What is Critical Thinking in Nursing? (With Examples, Importance, & How to Improve)

Successful nursing requires learning several skills used to communicate with patients, families, and healthcare teams. One of the most essential skills nurses must develop is the ability to demonstrate critical thinking. If you are a nurse, perhaps you have asked if there is a way to know how to improve critical thinking in nursing? As you read this article, you will learn what critical thinking in nursing is and why it is important. You will also find 18 simple tips to improve critical thinking in nursing and sample scenarios about how to apply critical thinking in your nursing career.

What is Critical Thinking in Nursing?
4 reasons why critical thinking is so important in nursing, 1. critical thinking skills will help you anticipate and understand changes in your patient’s condition., 2. with strong critical thinking skills, you can make decisions about patient care that is most favorable for the patient and intended outcomes., 3. strong critical thinking skills in nursing can contribute to innovative improvements and professional development., 4. critical thinking skills in nursing contribute to rational decision-making, which improves patient outcomes., what are the 8 important attributes of excellent critical thinking in nursing, 1. the ability to interpret information:, 2. independent thought:, 3. impartiality:, 4. intuition:, 5. problem solving:, 6. flexibility:, 7. perseverance:, 8. integrity:, examples of poor critical thinking vs excellent critical thinking in nursing, 1. scenario: patient/caregiver interactions, poor critical thinking:, excellent critical thinking:, 2. scenario: improving patient care quality, 3. scenario: interdisciplinary collaboration, 4. scenario: precepting nursing students and other nurses, how to improve critical thinking in nursing, 1. demonstrate open-mindedness., 2. practice self-awareness., 3. avoid judgment., 4. eliminate personal biases., 5. do not be afraid to ask questions., 6. find an experienced mentor., 7. join professional nursing organizations., 8. establish a routine of self-reflection., 9. utilize the chain of command., 10. determine the significance of data and decide if it is sufficient for decision-making., 11. volunteer for leadership positions or opportunities., 12. use previous facts and experiences to help develop stronger critical thinking skills in nursing., 13. establish priorities., 14. trust your knowledge and be confident in your abilities., 15. be curious about everything., 16. practice fair-mindedness., 17. learn the value of intellectual humility., 18. never stop learning., 4 consequences of poor critical thinking in nursing, 1. the most significant risk associated with poor critical thinking in nursing is inadequate patient care., 2. failure to recognize changes in patient status:, 3. lack of effective critical thinking in nursing can impact the cost of healthcare., 4. lack of critical thinking skills in nursing can cause a breakdown in communication within the interdisciplinary team., useful resources to improve critical thinking in nursing, youtube videos, my final thoughts, frequently asked questions answered by our expert, 1. will lack of critical thinking impact my nursing career, 2. usually, how long does it take for a nurse to improve their critical thinking skills, 3. do all types of nurses require excellent critical thinking skills, 4. how can i assess my critical thinking skills in nursing.
• Ask relevant questions • Justify opinions • Address and evaluate multiple points of view • Explain assumptions and reasons related to your choice of patient care options
5. Can I Be a Nurse If I Cannot Think Critically?


What is Critical Thinking in Nursing? (Explained W/ Examples)

Last updated on August 23rd, 2023
Critical thinking is a foundational skill applicable across various domains, including education, problem-solving, decision-making, and professional fields such as science, business, healthcare, and more.
It plays a crucial role in promoting logical and rational thinking, fostering informed decision-making, and enabling individuals to navigate complex and rapidly changing environments.
In this article, we will look at what is critical thinking in nursing practice, its importance, and how it enables nurses to excel in their roles while also positively impacting patient outcomes.

What is Critical Thinking?
Critical thinking is a cognitive process that involves analyzing, evaluating, and synthesizing information to make reasoned and informed decisions.
It’s a mental activity that goes beyond simple memorization or acceptance of information at face value.
Critical thinking involves careful, reflective, and logical thinking to understand complex problems, consider various perspectives, and arrive at well-reasoned conclusions or solutions.
Key aspects of critical thinking include:
- Analysis: Critical thinking begins with the thorough examination of information, ideas, or situations. It involves breaking down complex concepts into smaller parts to better understand their components and relationships.
- Evaluation: Critical thinkers assess the quality and reliability of information or arguments. They weigh evidence, identify strengths and weaknesses, and determine the credibility of sources.
- Synthesis: Critical thinking involves combining different pieces of information or ideas to create a new understanding or perspective. This involves connecting the dots between various sources and integrating them into a coherent whole.
- Inference: Critical thinkers draw logical and well-supported conclusions based on the information and evidence available. They use reasoning to make educated guesses about situations where complete information might be lacking.
- Problem-Solving: Critical thinking is essential in solving complex problems. It allows individuals to identify and define problems, generate potential solutions, evaluate the pros and cons of each solution, and choose the most appropriate course of action.
- Creativity: Critical thinking involves thinking outside the box and considering alternative viewpoints or approaches. It encourages the exploration of new ideas and solutions beyond conventional thinking.
- Reflection: Critical thinkers engage in self-assessment and reflection on their thought processes. They consider their own biases, assumptions, and potential errors in reasoning, aiming to improve their thinking skills over time.
- Open-Mindedness: Critical thinkers approach ideas and information with an open mind, willing to consider different viewpoints and perspectives even if they challenge their own beliefs.
- Effective Communication: Critical thinkers can articulate their thoughts and reasoning clearly and persuasively to others. They can express complex ideas in a coherent and understandable manner.
- Continuous Learning: Critical thinking encourages a commitment to ongoing learning and intellectual growth. It involves seeking out new knowledge, refining thinking skills, and staying receptive to new information.
Definition of Critical Thinking
Critical thinking is an intellectual process of analyzing, evaluating, and synthesizing information to make reasoned and informed decisions.
What is Critical Thinking in Nursing?
Critical thinking in nursing is a vital cognitive skill that involves analyzing, evaluating, and making reasoned decisions about patient care.
It’s an essential aspect of a nurse’s professional practice as it enables them to provide safe and effective care to patients.
Critical thinking involves a careful and deliberate thought process to gather and assess information, consider alternative solutions, and make informed decisions based on evidence and sound judgment.
This skill helps nurses to:
- Assess Information: Critical thinking allows nurses to thoroughly assess patient information, including medical history, symptoms, and test results. By analyzing this data, nurses can identify patterns, discrepancies, and potential issues that may require further investigation.
- Diagnose: Nurses use critical thinking to analyze patient data and collaboratively work with other healthcare professionals to formulate accurate nursing diagnoses. This is crucial for developing appropriate care plans that address the unique needs of each patient.
- Plan and Implement Care: Once a nursing diagnosis is established, critical thinking helps nurses develop effective care plans. They consider various interventions and treatment options, considering the patient’s preferences, medical history, and evidence-based practices.
- Evaluate Outcomes: After implementing interventions, critical thinking enables nurses to evaluate the outcomes of their actions. If the desired outcomes are not achieved, nurses can adapt their approach and make necessary changes to the care plan.
- Prioritize Care: In busy healthcare environments, nurses often face situations where they must prioritize patient care. Critical thinking helps them determine which patients require immediate attention and which interventions are most essential.
- Communicate Effectively: Critical thinking skills allow nurses to communicate clearly and confidently with patients, their families, and other members of the healthcare team. They can explain complex medical information and treatment plans in a way that is easily understood by all parties involved.
- Identify Problems: Nurses use critical thinking to identify potential complications or problems in a patient’s condition. This early recognition can lead to timely interventions and prevent further deterioration.
- Collaborate: Healthcare is a collaborative effort involving various professionals. Critical thinking enables nurses to actively participate in interdisciplinary discussions, share their insights, and contribute to holistic patient care.
- Ethical Decision-Making: Critical thinking helps nurses navigate ethical dilemmas that can arise in patient care. They can analyze different perspectives, consider ethical principles, and make morally sound decisions.
- Continual Learning: Critical thinking encourages nurses to seek out new knowledge, stay up-to-date with the latest research and medical advancements, and incorporate evidence-based practices into their care.
In summary, critical thinking is an integral skill for nurses, allowing them to provide high-quality, patient-centered care by analyzing information, making informed decisions, and adapting their approaches as needed.
It’s a dynamic process that enhances clinical reasoning , problem-solving, and overall patient outcomes.
What are the Levels of Critical Thinking in Nursing?

The development of critical thinking in nursing practice involves progressing through three levels: basic, complex, and commitment.
The Kataoka-Yahiro and Saylor model outlines this progression.
1. Basic Critical Thinking:
At this level, learners trust experts for solutions. Thinking is based on rules and principles. For instance, nursing students may strictly follow a procedure manual without personalization, as they lack experience. Answers are seen as right or wrong, and the opinions of experts are accepted.
2. Complex Critical Thinking:
Learners start to analyze choices independently and think creatively. They recognize conflicting solutions and weigh benefits and risks. Thinking becomes innovative, with a willingness to consider various approaches in complex situations.
3. Commitment:
At this level, individuals anticipate decision points without external help and take responsibility for their choices. They choose actions or beliefs based on available alternatives, considering consequences and accountability.
As nurses gain knowledge and experience, their critical thinking evolves from relying on experts to independent analysis and decision-making, ultimately leading to committed and accountable choices in patient care.
Why Critical Thinking is Important in Nursing?
Critical thinking is important in nursing for several crucial reasons:
Patient Safety:
Nursing decisions directly impact patient well-being. Critical thinking helps nurses identify potential risks, make informed choices, and prevent errors.
Clinical Judgment:
Nursing decisions often involve evaluating information from various sources, such as patient history, lab results, and medical literature.
Critical thinking assists nurses in critically appraising this information, distinguishing credible sources, and making rational judgments that align with evidence-based practices.
Enhances Decision-Making:
In nursing, critical thinking allows nurses to gather relevant patient information, assess it objectively, and weigh different options based on evidence and analysis.
This process empowers them to make informed decisions about patient care, treatment plans, and interventions, ultimately leading to better outcomes.
Promotes Problem-Solving:
Nurses encounter complex patient issues that require effective problem-solving.
Critical thinking equips them to break down problems into manageable parts, analyze root causes, and explore creative solutions that consider the unique needs of each patient.
Drives Creativity:
Nursing care is not always straightforward. Critical thinking encourages nurses to think creatively and explore innovative approaches to challenges, especially when standard protocols might not suffice for unique patient situations.
Fosters Effective Communication:
Communication is central to nursing. Critical thinking enables nurses to clearly express their thoughts, provide logical explanations for their decisions, and engage in meaningful dialogues with patients, families, and other healthcare professionals.
Aids Learning:
Nursing is a field of continuous learning. Critical thinking encourages nurses to engage in ongoing self-directed education, seeking out new knowledge, embracing new techniques, and staying current with the latest research and developments.
Improves Relationships:
Open-mindedness and empathy are essential in nursing relationships.
Critical thinking encourages nurses to consider diverse viewpoints, understand patients’ perspectives, and communicate compassionately, leading to stronger therapeutic relationships.
Empowers Independence:
Nursing often requires autonomous decision-making. Critical thinking empowers nurses to analyze situations independently, make judgments without undue influence, and take responsibility for their actions.
Facilitates Adaptability:
Healthcare environments are ever-changing. Critical thinking equips nurses with the ability to quickly assess new information, adjust care plans, and navigate unexpected situations while maintaining patient safety and well-being.
Strengthens Critical Analysis:
In the era of vast information, nurses must discern reliable data from misinformation.
Critical thinking helps them scrutinize sources, question assumptions, and make well-founded choices based on credible information.
How to Apply Critical Thinking in Nursing? (With Examples)
Here are some examples of how nurses can apply critical thinking.
Assess Patient Data:
Critical Thinking Action: Carefully review patient history, symptoms, and test results.
Example: A nurse notices a change in a diabetic patient’s blood sugar levels. Instead of just administering insulin, the nurse considers recent dietary changes, activity levels, and possible medication interactions before adjusting the treatment plan.
Diagnose Patient Needs:
Critical Thinking Action: Analyze patient data to identify potential nursing diagnoses.
Example: After reviewing a patient’s lab results, vital signs, and observations, a nurse identifies “ Risk for Impaired Skin Integrity ” due to the patient’s limited mobility.
Plan and Implement Care:
Critical Thinking Action: Develop a care plan based on patient needs and evidence-based practices.
Example: For a patient at risk of falls, the nurse plans interventions such as hourly rounding, non-slip footwear, and bed alarms to ensure patient safety.
Evaluate Interventions:
Critical Thinking Action: Assess the effectiveness of interventions and modify the care plan as needed.
Example: After administering pain medication, the nurse evaluates its impact on the patient’s comfort level and considers adjusting the dosage or trying an alternative pain management approach.
Prioritize Care:
Critical Thinking Action: Determine the order of interventions based on patient acuity and needs.
Example: In a busy emergency department, the nurse triages patients by considering the severity of their conditions, ensuring that critical cases receive immediate attention.
Collaborate with the Healthcare Team:
Critical Thinking Action: Participate in interdisciplinary discussions and share insights.
Example: During rounds, a nurse provides input on a patient’s response to treatment, which prompts the team to adjust the care plan for better outcomes.
Ethical Decision-Making:
Critical Thinking Action: Analyze ethical dilemmas and make morally sound choices.
Example: When a terminally ill patient expresses a desire to stop treatment, the nurse engages in ethical discussions, respecting the patient’s autonomy and ensuring proper end-of-life care.
Patient Education:
Critical Thinking Action: Tailor patient education to individual needs and comprehension levels.
Example: A nurse uses visual aids and simplified language to explain medication administration to a patient with limited literacy skills.
Adapt to Changes:
Critical Thinking Action: Quickly adjust care plans when patient conditions change.
Example: During post-operative recovery, a nurse notices signs of infection and promptly informs the healthcare team to initiate appropriate treatment adjustments.
Critical Analysis of Information:
Critical Thinking Action: Evaluate information sources for reliability and relevance.
Example: When presented with conflicting research studies, a nurse critically examines the methodologies and sample sizes to determine which study is more credible.
Making Sense of Critical Thinking Skills
What is the purpose of critical thinking in nursing.
The purpose of critical thinking in nursing is to enable nurses to effectively analyze, interpret, and evaluate patient information, make informed clinical judgments, develop appropriate care plans, prioritize interventions, and adapt their approaches as needed, thereby ensuring safe, evidence-based, and patient-centered care.
Why critical thinking is important in nursing?
Critical thinking is important in nursing because it promotes safe decision-making, accurate clinical judgment, problem-solving, evidence-based practice, holistic patient care, ethical reasoning, collaboration, and adapting to dynamic healthcare environments.
Critical thinking skill also enhances patient safety, improves outcomes, and supports nurses’ professional growth.
How is critical thinking used in the nursing process?
Critical thinking is integral to the nursing process as it guides nurses through the systematic approach of assessing, diagnosing, planning, implementing, and evaluating patient care. It involves:
- Assessment: Critical thinking enables nurses to gather and interpret patient data accurately, recognizing relevant patterns and cues.
- Diagnosis: Nurses use critical thinking to analyze patient data, identify nursing diagnoses, and differentiate actual issues from potential complications.
- Planning: Critical thinking helps nurses develop tailored care plans, selecting appropriate interventions based on patient needs and evidence.
- Implementation: Nurses make informed decisions during interventions, considering patient responses and adjusting plans as needed.
- Evaluation: Critical thinking supports the assessment of patient outcomes, determining the effectiveness of intervention, and adapting care accordingly.
Throughout the nursing process , critical thinking ensures comprehensive, patient-centered care and fosters continuous improvement in clinical judgment and decision-making.
What is an example of the critical thinking attitude of independent thinking in nursing practice?
An example of the critical thinking attitude of independent thinking in nursing practice could be:
A nurse is caring for a patient with a complex medical history who is experiencing a new set of symptoms. The nurse carefully reviews the patient’s history, recent test results, and medication list.
While discussing the case with the healthcare team, the nurse realizes that the current treatment plan might not be addressing all aspects of the patient’s condition.
Instead of simply following the established protocol, the nurse independently considers alternative approaches based on their assessment.
The nurse proposes a modification to the treatment plan, citing the rationale and evidence supporting the change.
This demonstrates independent thinking by critically evaluating the situation, challenging assumptions, and advocating for a more personalized and effective patient care approach.
How to use Costa’s level of questioning for critical thinking in nursing?
Costa’s levels of questioning can be applied in nursing to facilitate critical thinking and stimulate a deeper understanding of patient situations. The levels of questioning are as follows:
| Level 1: Gathering | 1. What are the common side effects of the prescribed medication? 2. When was the patient’s last bowel movement? 3. Who is the patient’s emergency contact person? 4. Describe the patient’s current level of pain. 5. What information is in the patient’s medical record? |
| 1. What would happen if the patient’s blood pressure falls further? 2. Compare the patient’s oxygen saturation levels before and after administering oxygen. 3. What other nursing interventions could be considered for wound care? 4. Infer the potential reasons behind the patient’s increased heart rate. 5. Analyze the relationship between the patient’s diet and blood glucose levels. | |
| 1. What do you think will be the patient’s response to the new pain management strategy? 2. Could the patient’s current symptoms be indicative of an underlying complication? 3. How would you prioritize care for patients with varying acuity levels in the emergency department? 4. What evidence supports your choice of administering the medication at this time? 5. Create a care plan for a patient with complex needs requiring multiple interventions. |
- 15 Attitudes of Critical Thinking in Nursing (Explained W/ Examples)
- Nursing Concept Map (FREE Template)
- Clinical Reasoning In Nursing (Explained W/ Example)
- 8 Stages Of The Clinical Reasoning Cycle
- How To Improve Critical Thinking Skills In Nursing? 24 Strategies With Examples
- What is the “5 Whys” Technique?
- What Are Socratic Questions?
Critical thinking in nursing is the foundation that underpins safe, effective, and patient-centered care.
Critical thinking skills empower nurses to navigate the complexities of their profession while consistently providing high-quality care to diverse patient populations.
Reading Recommendation
Potter, P.A., Perry, A.G., Stockert, P. and Hall, A. (2013) Fundamentals of Nursing
Comments are closed.
Medical & Legal Disclaimer
All the contents on this site are for entertainment, informational, educational, and example purposes ONLY. These contents are not intended to be used as a substitute for professional medical advice or practice guidelines. However, we aim to publish precise and current information. By using any content on this website, you agree never to hold us legally liable for damages, harm, loss, or misinformation. Read the privacy policy and terms and conditions.
Privacy Policy
Terms & Conditions
© 2024 nurseship.com. All rights reserved.
Critical Thinking and the Nursing Process
In today’s health care arena, the nurse is faced with increasingly complex issues and situations resulting from advanced technology, greater acuity of patients in hospital and community settings, an aging population, and complex disease processes, as well as ethical and cultural factors. Traditionally, nurses have used a problem-solving approach in planning and providing nursing care. Today the decision-making part of problem solving has become increasingly complex and requires critical thinking.
Definition of Critical thinking
Critical thinking is a multidimensional skill, a cognitive or mental process or set of procedures. It involves reasoning and purposeful, systematic, reflective, rational, outcome-directed thinking based on a body of knowledge, as well as examination and analysis of all available information and ideas. Critical thinking leads to the formulation of conclusions and the most appropriate, often creative, decisions, options, or alternatives. Critical thinking includes metacognition, the examination of one’s own reasoning or thought processes while thinking, to help strengthen and refine thinking skills. Independent judgments and decisions evolve from a sound knowledge base and the ability to synthesize information within the context in which it is presented. Nursing practice in today’s society mandates the use of high-level critical thinking skills within the nursing process. Critical thinking enhances clinical decision making, helping to identify patient needs and to determine the best nursing actions that will assist the patient in meeting those needs. Critical thinking and critical thinkers have distinctive characteristics. As indicated in the above definition, critical thinking is a conscious, outcome-oriented activity; it is purposeful and intentional. The critical thinker is an inquisitive, fair-minded truth seeker with an open-mindedness to the alternative solutions that might surface.
Critical thinking Process: Rationality and Insight
Critical thinking is systematic and organized. The skills involved in critical thinking are developed over time through effort, practice, and experience. Skills needed in critical thinking include interpretation, analysis, evaluation, inference, explanation, and self-regulation. Critical thinking requires background knowledge and knowledge of key concepts as well as standards of good thinking. The critical thinker uses reality-based deliberation to validate the accuracy of data and the reliability of sources, being mindful of and questioning inconsistencies. Interpretation is used to determine the significance of data that are gathered, and analysis is used to identify patient problems indicated by the data. The nurse uses inference to draw conclusions. Explanation is the justification of actions or interventions used to address patient problems and to help a patient move toward desired outcomes. Evaluation is the process of determining whether outcomes have been or are being met, and self-regulation is the process of examining the care provided and adjusting the interventions as needed. Critical thinking is also reflective, involving metacognition, active evaluation, and refinement of the thinking process. The critical thinker considers the possibility of personal bias when interpreting data and determining appropriate actions. The critical thinker must be insightful and have a sense of fairness and integrity, the courage to question personal ethics, and the perseverance to strive continuously to minimize the effects of egocentricity, ethnocentricity, and other biases on the decision making process.
Components of Critical thinking
Certain cognitive or mental activities can be identified as key components of critical thinking. When thinking critically, a person will do the following:
- Ask questions to determine the reason why certain developments have occurred and to see whether more information is needed to understand the situation accurately.
- Gather as much relevant information as possible to consider as many factors as possible.
- Validate the information presented to make sure that it is accurate (not just supposition or opinion), that it makes sense, and that it is based on fact and evidence.
- Analyze the information to determine what it means and to see whether it forms clusters or patterns that point to certain conclusions.
- Draw on past clinical experience and knowledge to explain what is happening and to anticipate what might happen next, acknowledging personal bias and cultural influences.
- Maintain a flexible attitude that allows the facts to guide thinking and takes into account all possibilities.
- Consider available options and examine each in terms of its advantages and disadvantages.
- Formulate decisions that reflect creativity and independent decision making.
Critical thinking requires going beyond basic problem solving into a realm of inquisitive exploration, looking for all relevant factors that affect the issue, and being an “out-of-the-box” thinker. It includes questioning all findings until a comprehensive picture emerges that explains the phenomenon, possible solutions, and creative methods for proceeding. Critical thinking in nursing practice results in a comprehensive patient plan of care with maximized potential for success.
Critical thinking In Nursing Practice
Using critical thinking to develop a plan of nursing care requires considering the human factors that might influence the plan. The nurse interacts with the patient, family, and other health care providers in the process of providing appropriate, individualized nursing care. The culture, attitude, and thought processes of the nurse, the patient, and others will affect the critical thinking process from the data-gathering stage through the decision-making stage; therefore, aspects of the nurse-patient interaction must be considered. Nurses must use critical thinking skills in all practice settings—acute care, ambulatory care, extended care, and in the home and community. Regardless of the setting, each patient situation is viewed as unique and dynamic. The unique factors that the patient and nurse bring to the health care situation are considered, studied, analyzed, and interpreted. Interpretation of the information presented then allows the nurse to focus on those factors that are most relevant and mostsignificant to the clinical situation. Decisions about what to do and how to do it are then developed into a plan of action.
Fonteyn (1998) identified 12 predominant thinking strategies used by nurses, regardless of their area of clinical practice:
Recognizing a pattern
- Setting priorities
- Searching for information
- Generating hypotheses
- Making predictions
- Forming relationships
- Stating a proposition (“if–then”)
- Asserting a practice rule
- Making choices (alternative actions)
- Judging the value
- Drawing conclusions
- Providing explanations
Fonteyn further identified other, less prominent thinking strategies the nurse might use:
- Posing a question
- Making assumptions (supposing)
- Making generalizations
These thought processes are consistent with the characteristics of critical thinking and cognitive activities discussed earlier. Fonteyn asserted that exploring how these thinking strategies are used in various clinical situations, and practicing using the strategies, might assist the nurse–learner in examining and refining his or her own thinking skills.
Throughout the critical thinking process, a continuous flow of questions evolves in the thinker’s mind. Although the questions will vary according to the particular clinical situation, certain general inquiries can serve as a basis for reaching conclusions and determining a course of action. When faced with a patient situation, it is often helpful to seek answers to some or all of the following questions in an attempt to determine those actions that are most appropriate:
- What relevant assessment information do I need, and how do I interpret this information? What does this information tell me?
- To what problems does this information point? Have I identified the most important ones? Does the information point to any other problems that I should consider?
- Have I gathered all the information I need (signs/symptoms, laboratory values, medication history, emotional factors, mental status)? Is anything missing?
- Is there anything that needs to be reported immediately? Do I need to seek additional assistance?
- Does this patient have any special risk factors? Which ones are most significant? What must I do to minimize these risks?
- What possible complications must I anticipate?
- What are the most important problems in this situation? Do the patient and the patient’s family recognize the same problems?
- What are the desired outcomes for this patient? Which have the highest priority? Does the patient see eye to eye with me on these points?
- What is going to be my first action in this situation? How can I construct a plan of care to achieve the goals?
- Are there any age-related factors involved, and will they require some special approach? Will I need to make some change in the plan of care to take these factors into account?
- How do the family dynamics affect this situation, and will this have an affect on my actions or the plan of care?
- Are there cultural factors that I must address and consider?
- Am I dealing with an ethical problem here? If so, how am I going to resolve it?
- Has any nursing research been conducted on this subject?
Related Posts
Cleaning bedpans and urinals, teaching people with disabilities, assessment – first step in the nursing process.
The Value of Critical Thinking in Nursing

- How Nurses Use Critical Thinking
- How to Improve Critical Thinking
- Common Mistakes

Some experts describe a person’s ability to question belief systems, test previously held assumptions, and recognize ambiguity as evidence of critical thinking. Others identify specific skills that demonstrate critical thinking, such as the ability to identify problems and biases, infer and draw conclusions, and determine the relevance of information to a situation.
Nicholas McGowan, BSN, RN, CCRN, has been a critical care nurse for 10 years in neurological trauma nursing and cardiovascular and surgical intensive care. He defines critical thinking as “necessary for problem-solving and decision-making by healthcare providers. It is a process where people use a logical process to gather information and take purposeful action based on their evaluation.”
“This cognitive process is vital for excellent patient outcomes because it requires that nurses make clinical decisions utilizing a variety of different lenses, such as fairness, ethics, and evidence-based practice,” he says.
How Do Nurses Use Critical Thinking?
Successful nurses think beyond their assigned tasks to deliver excellent care for their patients. For example, a nurse might be tasked with changing a wound dressing, delivering medications, and monitoring vital signs during a shift. However, it requires critical thinking skills to understand how a difference in the wound may affect blood pressure and temperature and when those changes may require immediate medical intervention.
Nurses care for many patients during their shifts. Strong critical thinking skills are crucial when juggling various tasks so patient safety and care are not compromised.
Jenna Liphart Rhoads, Ph.D., RN, is a nurse educator with a clinical background in surgical-trauma adult critical care, where critical thinking and action were essential to the safety of her patients. She talks about examples of critical thinking in a healthcare environment, saying:
“Nurses must also critically think to determine which patient to see first, which medications to pass first, and the order in which to organize their day caring for patients. Patient conditions and environments are continually in flux, therefore nurses must constantly be evaluating and re-evaluating information they gather (assess) to keep their patients safe.”
The COVID-19 pandemic created hospital care situations where critical thinking was essential. It was expected of the nurses on the general floor and in intensive care units. Crystal Slaughter is an advanced practice nurse in the intensive care unit (ICU) and a nurse educator. She observed critical thinking throughout the pandemic as she watched intensive care nurses test the boundaries of previously held beliefs and master providing excellent care while preserving resources.
“Nurses are at the patient’s bedside and are often the first ones to detect issues. Then, the nurse needs to gather the appropriate subjective and objective data from the patient in order to frame a concise problem statement or question for the physician or advanced practice provider,” she explains.
Top 5 Ways Nurses Can Improve Critical Thinking Skills
We asked our experts for the top five strategies nurses can use to purposefully improve their critical thinking skills.
Case-Based Approach
Slaughter is a fan of the case-based approach to learning critical thinking skills.
In much the same way a detective would approach a mystery, she mentors her students to ask questions about the situation that help determine the information they have and the information they need. “What is going on? What information am I missing? Can I get that information? What does that information mean for the patient? How quickly do I need to act?”
Consider forming a group and working with a mentor who can guide you through case studies. This provides you with a learner-centered environment in which you can analyze data to reach conclusions and develop communication, analytical, and collaborative skills with your colleagues.
Practice Self-Reflection
Rhoads is an advocate for self-reflection. “Nurses should reflect upon what went well or did not go well in their workday and identify areas of improvement or situations in which they should have reached out for help.” Self-reflection is a form of personal analysis to observe and evaluate situations and how you responded.
This gives you the opportunity to discover mistakes you may have made and to establish new behavior patterns that may help you make better decisions. You likely already do this. For example, after a disagreement or contentious meeting, you may go over the conversation in your head and think about ways you could have responded.
It’s important to go through the decisions you made during your day and determine if you should have gotten more information before acting or if you could have asked better questions.
During self-reflection, you may try thinking about the problem in reverse. This may not give you an immediate answer, but can help you see the situation with fresh eyes and a new perspective. How would the outcome of the day be different if you planned the dressing change in reverse with the assumption you would find a wound infection? How does this information change your plan for the next dressing change?
Develop a Questioning Mind
McGowan has learned that “critical thinking is a self-driven process. It isn’t something that can simply be taught. Rather, it is something that you practice and cultivate with experience. To develop critical thinking skills, you have to be curious and inquisitive.”
To gain critical thinking skills, you must undergo a purposeful process of learning strategies and using them consistently so they become a habit. One of those strategies is developing a questioning mind. Meaningful questions lead to useful answers and are at the core of critical thinking .
However, learning to ask insightful questions is a skill you must develop. Faced with staff and nursing shortages , declining patient conditions, and a rising number of tasks to be completed, it may be difficult to do more than finish the task in front of you. Yet, questions drive active learning and train your brain to see the world differently and take nothing for granted.
It is easier to practice questioning in a non-stressful, quiet environment until it becomes a habit. Then, in the moment when your patient’s care depends on your ability to ask the right questions, you can be ready to rise to the occasion.
Practice Self-Awareness in the Moment
Critical thinking in nursing requires self-awareness and being present in the moment. During a hectic shift, it is easy to lose focus as you struggle to finish every task needed for your patients. Passing medication, changing dressings, and hanging intravenous lines all while trying to assess your patient’s mental and emotional status can affect your focus and how you manage stress as a nurse .
Staying present helps you to be proactive in your thinking and anticipate what might happen, such as bringing extra lubricant for a catheterization or extra gloves for a dressing change.
By staying present, you are also better able to practice active listening. This raises your assessment skills and gives you more information as a basis for your interventions and decisions.
Use a Process
As you are developing critical thinking skills, it can be helpful to use a process. For example:
- Ask questions.
- Gather information.
- Implement a strategy.
- Evaluate the results.
- Consider another point of view.
These are the fundamental steps of the nursing process (assess, diagnose, plan, implement, evaluate). The last step will help you overcome one of the common problems of critical thinking in nursing — personal bias.
Common Critical Thinking Pitfalls in Nursing
Your brain uses a set of processes to make inferences about what’s happening around you. In some cases, your unreliable biases can lead you down the wrong path. McGowan places personal biases at the top of his list of common pitfalls to critical thinking in nursing.
“We all form biases based on our own experiences. However, nurses have to learn to separate their own biases from each patient encounter to avoid making false assumptions that may interfere with their care,” he says. Successful critical thinkers accept they have personal biases and learn to look out for them. Awareness of your biases is the first step to understanding if your personal bias is contributing to the wrong decision.
New nurses may be overwhelmed by the transition from academics to clinical practice, leading to a task-oriented mindset and a common new nurse mistake ; this conflicts with critical thinking skills.
“Consider a patient whose blood pressure is low but who also needs to take a blood pressure medication at a scheduled time. A task-oriented nurse may provide the medication without regard for the patient’s blood pressure because medication administration is a task that must be completed,” Slaughter says. “A nurse employing critical thinking skills would address the low blood pressure, review the patient’s blood pressure history and trends, and potentially call the physician to discuss whether medication should be withheld.”
Fear and pride may also stand in the way of developing critical thinking skills. Your belief system and worldview provide comfort and guidance, but this can impede your judgment when you are faced with an individual whose belief system or cultural practices are not the same as yours. Fear or pride may prevent you from pursuing a line of questioning that would benefit the patient. Nurses with strong critical thinking skills exhibit:
- Learn from their mistakes and the mistakes of other nurses
- Look forward to integrating changes that improve patient care
- Treat each patient interaction as a part of a whole
- Evaluate new events based on past knowledge and adjust decision-making as needed
- Solve problems with their colleagues
- Are self-confident
- Acknowledge biases and seek to ensure these do not impact patient care
An Essential Skill for All Nurses
Critical thinking in nursing protects patient health and contributes to professional development and career advancement. Administrative and clinical nursing leaders are required to have strong critical thinking skills to be successful in their positions.
By using the strategies in this guide during your daily life and in your nursing role, you can intentionally improve your critical thinking abilities and be rewarded with better patient outcomes and potential career advancement.
Frequently Asked Questions About Critical Thinking in Nursing
How are critical thinking skills utilized in nursing practice.
Nursing practice utilizes critical thinking skills to provide the best care for patients. Often, the patient’s cause of pain or health issue is not immediately clear. Nursing professionals need to use their knowledge to determine what might be causing distress, collect vital information, and make quick decisions on how best to handle the situation.
How does nursing school develop critical thinking skills?
Nursing school gives students the knowledge professional nurses use to make important healthcare decisions for their patients. Students learn about diseases, anatomy, and physiology, and how to improve the patient’s overall well-being. Learners also participate in supervised clinical experiences, where they practice using their critical thinking skills to make decisions in professional settings.
Do only nurse managers use critical thinking?
Nurse managers certainly use critical thinking skills in their daily duties. But when working in a health setting, anyone giving care to patients uses their critical thinking skills. Everyone — including licensed practical nurses, registered nurses, and advanced nurse practitioners —needs to flex their critical thinking skills to make potentially life-saving decisions.
Meet Our Contributors

Crystal Slaughter, DNP, APRN, ACNS-BC, CNE
Crystal Slaughter is a core faculty member in Walden University’s RN-to-BSN program. She has worked as an advanced practice registered nurse with an intensivist/pulmonary service to provide care to hospitalized ICU patients and in inpatient palliative care. Slaughter’s clinical interests lie in nursing education and evidence-based practice initiatives to promote improving patient care.

Jenna Liphart Rhoads, Ph.D., RN
Jenna Liphart Rhoads is a nurse educator and freelance author and editor. She earned a BSN from Saint Francis Medical Center College of Nursing and an MS in nursing education from Northern Illinois University. Rhoads earned a Ph.D. in education with a concentration in nursing education from Capella University where she researched the moderation effects of emotional intelligence on the relationship of stress and GPA in military veteran nursing students. Her clinical background includes surgical-trauma adult critical care, interventional radiology procedures, and conscious sedation in adult and pediatric populations.

Nicholas McGowan, BSN, RN, CCRN
Nicholas McGowan is a critical care nurse with 10 years of experience in cardiovascular, surgical intensive care, and neurological trauma nursing. McGowan also has a background in education, leadership, and public speaking. He is an online learner who builds on his foundation of critical care nursing, which he uses directly at the bedside where he still practices. In addition, McGowan hosts an online course at Critical Care Academy where he helps nurses achieve critical care (CCRN) certification.
An official website of the United States government
The .gov means it’s official. Federal government websites often end in .gov or .mil. Before sharing sensitive information, make sure you’re on a federal government site.
The site is secure. The https:// ensures that you are connecting to the official website and that any information you provide is encrypted and transmitted securely.
- Publications
- Account settings
- My Bibliography
- Collections
- Citation manager
Save citation to file
Email citation, add to collections.
- Create a new collection
- Add to an existing collection
Add to My Bibliography
Your saved search, create a file for external citation management software, your rss feed.
- Search in PubMed
- Search in NLM Catalog
- Add to Search
Critical thinking in nursing clinical practice, education and research: From attitudes to virtue
Affiliations.
- 1 Department of Fundamental Care and Medical Surgital Nursing, Faculty of Medicine and Health Sciences, School of Nursing, Consolidated Research Group Quantitative Psychology (2017-SGR-269), University of Barcelona, Barcelona, Spain.
- 2 Department of Fundamental Care and Medical Surgital Nursing, Faculty of Medicine and Health Sciences, School of Nursing, Consolidated Research Group on Gender, Identity and Diversity (2017-SGR-1091), University of Barcelona, Barcelona, Spain.
- 3 Department of Fundamental Care and Medical Surgital Nursing, Faculty of Medicine and Health Sciences, School of Nursing, University of Barcelona, Barcelona, Spain.
- 4 Multidisciplinary Nursing Research Group, Vall d'Hebron Research Institute (VHIR), Vall d'Hebron Hospital, Barcelona, Spain.
- PMID: 33029860
- DOI: 10.1111/nup.12332
Critical thinking is a complex, dynamic process formed by attitudes and strategic skills, with the aim of achieving a specific goal or objective. The attitudes, including the critical thinking attitudes, constitute an important part of the idea of good care, of the good professional. It could be said that they become a virtue of the nursing profession. In this context, the ethics of virtue is a theoretical framework that becomes essential for analyse the critical thinking concept in nursing care and nursing science. Because the ethics of virtue consider how cultivating virtues are necessary to understand and justify the decisions and guide the actions. Based on selective analysis of the descriptive and empirical literature that addresses conceptual review of critical thinking, we conducted an analysis of this topic in the settings of clinical practice, training and research from the virtue ethical framework. Following JBI critical appraisal checklist for text and opinion papers, we argue the need for critical thinking as an essential element for true excellence in care and that it should be encouraged among professionals. The importance of developing critical thinking skills in education is well substantiated; however, greater efforts are required to implement educational strategies directed at developing critical thinking in students and professionals undergoing training, along with measures that demonstrate their success. Lastly, we show that critical thinking constitutes a fundamental component in the research process, and can improve research competencies in nursing. We conclude that future research and actions must go further in the search for new evidence and open new horizons, to ensure a positive effect on clinical practice, patient health, student education and the growth of nursing science.
Keywords: critical thinking; critical thinking attitudes; nurse education; nursing care; nursing research.
© 2020 John Wiley & Sons Ltd.
PubMed Disclaimer
Similar articles
- Student and educator experiences of maternal-child simulation-based learning: a systematic review of qualitative evidence protocol. MacKinnon K, Marcellus L, Rivers J, Gordon C, Ryan M, Butcher D. MacKinnon K, et al. JBI Database System Rev Implement Rep. 2015 Jan;13(1):14-26. doi: 10.11124/jbisrir-2015-1694. JBI Database System Rev Implement Rep. 2015. PMID: 26447004
- Health professionals' experience of teamwork education in acute hospital settings: a systematic review of qualitative literature. Eddy K, Jordan Z, Stephenson M. Eddy K, et al. JBI Database System Rev Implement Rep. 2016 Apr;14(4):96-137. doi: 10.11124/JBISRIR-2016-1843. JBI Database System Rev Implement Rep. 2016. PMID: 27532314 Review.
- Strategies to overcome obstacles in the facilitation of critical thinking in nursing education. Mangena A, Chabeli MM. Mangena A, et al. Nurse Educ Today. 2005 May;25(4):291-8. doi: 10.1016/j.nedt.2005.01.012. Epub 2005 Apr 12. Nurse Educ Today. 2005. PMID: 15896414
- Ethics in nursing education: learning to reflect on care practices. Vanlaere L, Gastmans C. Vanlaere L, et al. Nurs Ethics. 2007 Nov;14(6):758-66. doi: 10.1177/0969733007082116. Nurs Ethics. 2007. PMID: 17901186 Review.
- Teaching strategies and outcome assessments targeting critical thinking in bachelor nursing students: a scoping review protocol. Westerdahl F, Carlson E, Wennick A, Borglin G. Westerdahl F, et al. BMJ Open. 2020 Feb 2;10(1):e033214. doi: 10.1136/bmjopen-2019-033214. BMJ Open. 2020. PMID: 32014875 Free PMC article. Review.
- Higher Vocational Nursing Students' Clinical Core Competence in China: A Cross-Sectional Study. Wang S, Huang S, Yan L. Wang S, et al. SAGE Open Nurs. 2024 Mar 1;10:23779608241233147. doi: 10.1177/23779608241233147. eCollection 2024 Jan-Dec. SAGE Open Nurs. 2024. PMID: 38435341 Free PMC article.
- Effect of the case-based learning method combined with virtual reality simulation technology on midwifery laboratory courses: A quasi-experimental study. Zhao L, Dai X, Chen S. Zhao L, et al. Int J Nurs Sci. 2023 Dec 16;11(1):76-82. doi: 10.1016/j.ijnss.2023.12.009. eCollection 2024 Jan. Int J Nurs Sci. 2023. PMID: 38352279 Free PMC article.
- Translation, validation and psychometric properties of the Albanian version of the Nurses Professional Competence Scale Short form. Duka B, Stievano A, Caruso R, Prendi E, Ejupi V, Spada F, De Maria M, Rocco G, Notarnicola I. Duka B, et al. Acta Biomed. 2023 Aug 3;94(4):e2023197. doi: 10.23750/abm.v94i4.13575. Acta Biomed. 2023. PMID: 37539614 Free PMC article.
- A study of the effects of blended learning on university students' critical thinking: A systematic review. Haftador AM, Tehranineshat B, Keshtkaran Z, Mohebbi Z. Haftador AM, et al. J Educ Health Promot. 2023 Mar 31;12:95. doi: 10.4103/jehp.jehp_665_22. eCollection 2023. J Educ Health Promot. 2023. PMID: 37288404 Free PMC article. Review.
- Multilevel Modeling of Individual and Group Level Influences on Critical Thinking and Clinical Decision-Making Skills among Registered Nurses: A Study Protocol. Zainal NH, Musa KI, Rasudin NS, Mamat Z. Zainal NH, et al. Healthcare (Basel). 2023 Apr 19;11(8):1169. doi: 10.3390/healthcare11081169. Healthcare (Basel). 2023. PMID: 37108003 Free PMC article.
- Alfaro-Lefevre, R. (2019). Critical thinking, clinical reasoning and clinical judgment. A practical approach, 7th ed. Elsevier.
- Armstrong, A. (2006). Towards a strong virtue ethics for nursing practice. Nursing Philosophy, 7(3), 110-124.
- Armstrong, A. (2007). Nursing ethics. A virtue-based approach. Palgrave Macmillian.
- Banks-Wallace, J., Despins, L., Adams-Leander, S., McBroom, L., & Tandy, L. (2008). Re/Affirming and re/conceptualizing disciplinary knowledge as the foundations for doctoral education. Advances in Nursing Sciencies, 31(1), 67-78. https://doi.org/10.1097/01.ANS.0000311530.81188.88
- Banning, M. (2008). Clinical reasoning and its application to nursing: Concepts and research studies. Nurse Education in Practice, 8(3), 177-183.
- Search in MeSH
Grants and funding
- PREI-19-007-B/School of Nursing. Faculty of Medicine and Health Sciences. University of Barcelona
LinkOut - more resources
Full text sources.
- Ovid Technologies, Inc.

- Citation Manager
NCBI Literature Resources
MeSH PMC Bookshelf Disclaimer
The PubMed wordmark and PubMed logo are registered trademarks of the U.S. Department of Health and Human Services (HHS). Unauthorized use of these marks is strictly prohibited.
- Visit Nurse.com on Facebook
- Visit Nurse.com on YouTube
- Visit Nurse.com on Instagram
- Visit Nurse.com on LinkedIn
Nurse.com by Relias . © Relias LLC 2024. All Rights Reserved.
Warning: The NCBI web site requires JavaScript to function. more...
An official website of the United States government
The .gov means it's official. Federal government websites often end in .gov or .mil. Before sharing sensitive information, make sure you're on a federal government site.
The site is secure. The https:// ensures that you are connecting to the official website and that any information you provide is encrypted and transmitted securely.
- Publications
- Account settings
- Browse Titles
NCBI Bookshelf. A service of the National Library of Medicine, National Institutes of Health.
Hughes RG, editor. Patient Safety and Quality: An Evidence-Based Handbook for Nurses. Rockville (MD): Agency for Healthcare Research and Quality (US); 2008 Apr.

Patient Safety and Quality: An Evidence-Based Handbook for Nurses.
Chapter 6 clinical reasoning, decisionmaking, and action: thinking critically and clinically.
Patricia Benner ; Ronda G. Hughes ; Molly Sutphen .
Affiliations
This chapter examines multiple thinking strategies that are needed for high-quality clinical practice. Clinical reasoning and judgment are examined in relation to other modes of thinking used by clinical nurses in providing quality health care to patients that avoids adverse events and patient harm. The clinician’s ability to provide safe, high-quality care can be dependent upon their ability to reason, think, and judge, which can be limited by lack of experience. The expert performance of nurses is dependent upon continual learning and evaluation of performance.
- Critical Thinking
Nursing education has emphasized critical thinking as an essential nursing skill for more than 50 years. 1 The definitions of critical thinking have evolved over the years. There are several key definitions for critical thinking to consider. The American Philosophical Association (APA) defined critical thinking as purposeful, self-regulatory judgment that uses cognitive tools such as interpretation, analysis, evaluation, inference, and explanation of the evidential, conceptual, methodological, criteriological, or contextual considerations on which judgment is based. 2 A more expansive general definition of critical thinking is
. . . in short, self-directed, self-disciplined, self-monitored, and self-corrective thinking. It presupposes assent to rigorous standards of excellence and mindful command of their use. It entails effective communication and problem solving abilities and a commitment to overcome our native egocentrism and sociocentrism. Every clinician must develop rigorous habits of critical thinking, but they cannot escape completely the situatedness and structures of the clinical traditions and practices in which they must make decisions and act quickly in specific clinical situations. 3
There are three key definitions for nursing, which differ slightly. Bittner and Tobin defined critical thinking as being “influenced by knowledge and experience, using strategies such as reflective thinking as a part of learning to identify the issues and opportunities, and holistically synthesize the information in nursing practice” 4 (p. 268). Scheffer and Rubenfeld 5 expanded on the APA definition for nurses through a consensus process, resulting in the following definition:
Critical thinking in nursing is an essential component of professional accountability and quality nursing care. Critical thinkers in nursing exhibit these habits of the mind: confidence, contextual perspective, creativity, flexibility, inquisitiveness, intellectual integrity, intuition, openmindedness, perseverance, and reflection. Critical thinkers in nursing practice the cognitive skills of analyzing, applying standards, discriminating, information seeking, logical reasoning, predicting, and transforming knowledge 6 (Scheffer & Rubenfeld, p. 357).
The National League for Nursing Accreditation Commission (NLNAC) defined critical thinking as:
the deliberate nonlinear process of collecting, interpreting, analyzing, drawing conclusions about, presenting, and evaluating information that is both factually and belief based. This is demonstrated in nursing by clinical judgment, which includes ethical, diagnostic, and therapeutic dimensions and research 7 (p. 8).
These concepts are furthered by the American Association of Colleges of Nurses’ definition of critical thinking in their Essentials of Baccalaureate Nursing :
Critical thinking underlies independent and interdependent decision making. Critical thinking includes questioning, analysis, synthesis, interpretation, inference, inductive and deductive reasoning, intuition, application, and creativity 8 (p. 9).
Course work or ethical experiences should provide the graduate with the knowledge and skills to:
- Use nursing and other appropriate theories and models, and an appropriate ethical framework;
- Apply research-based knowledge from nursing and the sciences as the basis for practice;
- Use clinical judgment and decision-making skills;
- Engage in self-reflective and collegial dialogue about professional practice;
- Evaluate nursing care outcomes through the acquisition of data and the questioning of inconsistencies, allowing for the revision of actions and goals;
- Engage in creative problem solving 8 (p. 10).
Taken together, these definitions of critical thinking set forth the scope and key elements of thought processes involved in providing clinical care. Exactly how critical thinking is defined will influence how it is taught and to what standard of care nurses will be held accountable.
Professional and regulatory bodies in nursing education have required that critical thinking be central to all nursing curricula, but they have not adequately distinguished critical reflection from ethical, clinical, or even creative thinking for decisionmaking or actions required by the clinician. Other essential modes of thought such as clinical reasoning, evaluation of evidence, creative thinking, or the application of well-established standards of practice—all distinct from critical reflection—have been subsumed under the rubric of critical thinking. In the nursing education literature, clinical reasoning and judgment are often conflated with critical thinking. The accrediting bodies and nursing scholars have included decisionmaking and action-oriented, practical, ethical, and clinical reasoning in the rubric of critical reflection and thinking. One might say that this harmless semantic confusion is corrected by actual practices, except that students need to understand the distinctions between critical reflection and clinical reasoning, and they need to learn to discern when each is better suited, just as students need to also engage in applying standards, evidence-based practices, and creative thinking.
The growing body of research, patient acuity, and complexity of care demand higher-order thinking skills. Critical thinking involves the application of knowledge and experience to identify patient problems and to direct clinical judgments and actions that result in positive patient outcomes. These skills can be cultivated by educators who display the virtues of critical thinking, including independence of thought, intellectual curiosity, courage, humility, empathy, integrity, perseverance, and fair-mindedness. 9
The process of critical thinking is stimulated by integrating the essential knowledge, experiences, and clinical reasoning that support professional practice. The emerging paradigm for clinical thinking and cognition is that it is social and dialogical rather than monological and individual. 10–12 Clinicians pool their wisdom and multiple perspectives, yet some clinical knowledge can be demonstrated only in the situation (e.g., how to suction an extremely fragile patient whose oxygen saturations sink too low). Early warnings of problematic situations are made possible by clinicians comparing their observations to that of other providers. Clinicians form practice communities that create styles of practice, including ways of doing things, communication styles and mechanisms, and shared expectations about performance and expertise of team members.
By holding up critical thinking as a large umbrella for different modes of thinking, students can easily misconstrue the logic and purposes of different modes of thinking. Clinicians and scientists alike need multiple thinking strategies, such as critical thinking, clinical judgment, diagnostic reasoning, deliberative rationality, scientific reasoning, dialogue, argument, creative thinking, and so on. In particular, clinicians need forethought and an ongoing grasp of a patient’s health status and care needs trajectory, which requires an assessment of their own clarity and understanding of the situation at hand, critical reflection, critical reasoning, and clinical judgment.
Critical Reflection, Critical Reasoning, and Judgment
Critical reflection requires that the thinker examine the underlying assumptions and radically question or doubt the validity of arguments, assertions, and even facts of the case. Critical reflective skills are essential for clinicians; however, these skills are not sufficient for the clinician who must decide how to act in particular situations and avoid patient injury. For example, in everyday practice, clinicians cannot afford to critically reflect on the well-established tenets of “normal” or “typical” human circulatory systems when trying to figure out a particular patient’s alterations from that typical, well-grounded understanding that has existed since Harvey’s work in 1628. 13 Yet critical reflection can generate new scientifically based ideas. For example, there is a lack of adequate research on the differences between women’s and men’s circulatory systems and the typical pathophysiology related to heart attacks. Available research is based upon multiple, taken-for-granted starting points about the general nature of the circulatory system. As such, critical reflection may not provide what is needed for a clinician to act in a situation. This idea can be considered reasonable since critical reflective thinking is not sufficient for good clinical reasoning and judgment. The clinician’s development of skillful critical reflection depends upon being taught what to pay attention to, and thus gaining a sense of salience that informs the powers of perceptual grasp. The powers of noticing or perceptual grasp depend upon noticing what is salient and the capacity to respond to the situation.
Critical reflection is a crucial professional skill, but it is not the only reasoning skill or logic clinicians require. The ability to think critically uses reflection, induction, deduction, analysis, challenging assumptions, and evaluation of data and information to guide decisionmaking. 9 , 14 , 15 Critical reasoning is a process whereby knowledge and experience are applied in considering multiple possibilities to achieve the desired goals, 16 while considering the patient’s situation. 14 It is a process where both inductive and deductive cognitive skills are used. 17 Sometimes clinical reasoning is presented as a form of evaluating scientific knowledge, sometimes even as a form of scientific reasoning. Critical thinking is inherent in making sound clinical reasoning. 18
An essential point of tension and confusion exists in practice traditions such as nursing and medicine when clinical reasoning and critical reflection become entangled, because the clinician must have some established bases that are not questioned when engaging in clinical decisions and actions, such as standing orders. The clinician must act in the particular situation and time with the best clinical and scientific knowledge available. The clinician cannot afford to indulge in either ritualistic unexamined knowledge or diagnostic or therapeutic nihilism caused by radical doubt, as in critical reflection, because they must find an intelligent and effective way to think and act in particular clinical situations. Critical reflection skills are essential to assist practitioners to rethink outmoded or even wrong-headed approaches to health care, health promotion, and prevention of illness and complications, especially when new evidence is available. Breakdowns in practice, high failure rates in particular therapies, new diseases, new scientific discoveries, and societal changes call for critical reflection about past assumptions and no-longer-tenable beliefs.
Clinical reasoning stands out as a situated, practice-based form of reasoning that requires a background of scientific and technological research-based knowledge about general cases, more so than any particular instance. It also requires practical ability to discern the relevance of the evidence behind general scientific and technical knowledge and how it applies to a particular patient. In dong so, the clinician considers the patient’s particular clinical trajectory, their concerns and preferences, and their particular vulnerabilities (e.g., having multiple comorbidities) and sensitivities to care interventions (e.g., known drug allergies, other conflicting comorbid conditions, incompatible therapies, and past responses to therapies) when forming clinical decisions or conclusions.
Situated in a practice setting, clinical reasoning occurs within social relationships or situations involving patient, family, community, and a team of health care providers. The expert clinician situates themselves within a nexus of relationships, with concerns that are bounded by the situation. Expert clinical reasoning is socially engaged with the relationships and concerns of those who are affected by the caregiving situation, and when certain circumstances are present, the adverse event. Halpern 19 has called excellent clinical ethical reasoning “emotional reasoning” in that the clinicians have emotional access to the patient/family concerns and their understanding of the particular care needs. Expert clinicians also seek an optimal perceptual grasp, one based on understanding and as undistorted as possible, based on an attuned emotional engagement and expert clinical knowledge. 19 , 20
Clergy educators 21 and nursing and medical educators have begun to recognize the wisdom of broadening their narrow vision of rationality beyond simple rational calculation (exemplified by cost-benefit analysis) to reconsider the need for character development—including emotional engagement, perception, habits of thought, and skill acquisition—as essential to the development of expert clinical reasoning, judgment, and action. 10 , 22–24 Practitioners of engineering, law, medicine, and nursing, like the clergy, have to develop a place to stand in their discipline’s tradition of knowledge and science in order to recognize and evaluate salient evidence in the moment. Diagnostic confusion and disciplinary nihilism are both threats to the clinician’s ability to act in particular situations. However, the practice and practitioners will not be self-improving and vital if they cannot engage in critical reflection on what is not of value, what is outmoded, and what does not work. As evidence evolves and expands, so too must clinical thought.
Clinical judgment requires clinical reasoning across time about the particular, and because of the relevance of this immediate historical unfolding, clinical reasoning can be very different from the scientific reasoning used to formulate, conduct, and assess clinical experiments. While scientific reasoning is also socially embedded in a nexus of social relationships and concerns, the goal of detached, critical objectivity used to conduct scientific experiments minimizes the interactive influence of the research on the experiment once it has begun. Scientific research in the natural and clinical sciences typically uses formal criteria to develop “yes” and “no” judgments at prespecified times. The scientist is always situated in past and immediate scientific history, preferring to evaluate static and predetermined points in time (e.g., snapshot reasoning), in contrast to a clinician who must always reason about transitions over time. 25 , 26
Techne and Phronesis
Distinctions between the mere scientific making of things and practice was first explored by Aristotle as distinctions between techne and phronesis. 27 Learning to be a good practitioner requires developing the requisite moral imagination for good practice. If, for example, patients exercise their rights and refuse treatments, practitioners are required to have the moral imagination to understand the probable basis for the patient’s refusal. For example, was the refusal based upon catastrophic thinking, unrealistic fears, misunderstanding, or even clinical depression?
Techne, as defined by Aristotle, encompasses the notion of formation of character and habitus 28 as embodied beings. In Aristotle’s terms, techne refers to the making of things or producing outcomes. 11 Joseph Dunne defines techne as “the activity of producing outcomes,” and it “is governed by a means-ends rationality where the maker or producer governs the thing or outcomes produced or made through gaining mastery over the means of producing the outcomes, to the point of being able to separate means and ends” 11 (p. 54). While some aspects of medical and nursing practice fall into the category of techne, much of nursing and medical practice falls outside means-ends rationality and must be governed by concern for doing good or what is best for the patient in particular circumstances, where being in a relationship and discerning particular human concerns at stake guide action.
Phronesis, in contrast to techne, includes reasoning about the particular, across time, through changes or transitions in the patient’s and/or the clinician’s understanding. As noted by Dunne, phronesis is “characterized at least as much by a perceptiveness with regard to concrete particulars as by a knowledge of universal principles” 11 (p. 273). This type of practical reasoning often takes the form of puzzle solving or the evaluation of immediate past “hot” history of the patient’s situation. Such a particular clinical situation is necessarily particular, even though many commonalities and similarities with other disease syndromes can be recognized through signs and symptoms and laboratory tests. 11 , 29 , 30 Pointing to knowledge embedded in a practice makes no claim for infallibility or “correctness.” Individual practitioners can be mistaken in their judgments because practices such as medicine and nursing are inherently underdetermined. 31
While phronetic knowledge must remain open to correction and improvement, real events, and consequences, it cannot consistently transcend the institutional setting’s capacities and supports for good practice. Phronesis is also dependent on ongoing experiential learning of the practitioner, where knowledge is refined, corrected, or refuted. The Western tradition, with the notable exception of Aristotle, valued knowledge that could be made universal and devalued practical know-how and experiential learning. Descartes codified this preference for formal logic and rational calculation.
Aristotle recognized that when knowledge is underdetermined, changeable, and particular, it cannot be turned into the universal or standardized. It must be perceived, discerned, and judged, all of which require experiential learning. In nursing and medicine, perceptual acuity in physical assessment and clinical judgment (i.e., reasoning across time about changes in the particular patient or the clinician’s understanding of the patient’s condition) fall into the Greek Aristotelian category of phronesis. Dewey 32 sought to rescue knowledge gained by practical activity in the world. He identified three flaws in the understanding of experience in Greek philosophy: (1) empirical knowing is the opposite of experience with science; (2) practice is reduced to techne or the application of rational thought or technique; and (3) action and skilled know-how are considered temporary and capricious as compared to reason, which the Greeks considered as ultimate reality.
In practice, nursing and medicine require both techne and phronesis. The clinician standardizes and routinizes what can be standardized and routinized, as exemplified by standardized blood pressure measurements, diagnoses, and even charting about the patient’s condition and treatment. 27 Procedural and scientific knowledge can often be formalized and standardized (e.g., practice guidelines), or at least made explicit and certain in practice, except for the necessary timing and adjustments made for particular patients. 11 , 22
Rational calculations available to techne—population trends and statistics, algorithms—are created as decision support structures and can improve accuracy when used as a stance of inquiry in making clinical judgments about particular patients. Aggregated evidence from clinical trials and ongoing working knowledge of pathophysiology, biochemistry, and genomics are essential. In addition, the skills of phronesis (clinical judgment that reasons across time, taking into account the transitions of the particular patient/family/community and transitions in the clinician’s understanding of the clinical situation) will be required for nursing, medicine, or any helping profession.
Thinking Critically
Being able to think critically enables nurses to meet the needs of patients within their context and considering their preferences; meet the needs of patients within the context of uncertainty; consider alternatives, resulting in higher-quality care; 33 and think reflectively, rather than simply accepting statements and performing tasks without significant understanding and evaluation. 34 Skillful practitioners can think critically because they have the following cognitive skills: information seeking, discriminating, analyzing, transforming knowledge, predicating, applying standards, and logical reasoning. 5 One’s ability to think critically can be affected by age, length of education (e.g., an associate vs. a baccalaureate decree in nursing), and completion of philosophy or logic subjects. 35–37 The skillful practitioner can think critically because of having the following characteristics: motivation, perseverance, fair-mindedness, and deliberate and careful attention to thinking. 5 , 9
Thinking critically implies that one has a knowledge base from which to reason and the ability to analyze and evaluate evidence. 38 Knowledge can be manifest by the logic and rational implications of decisionmaking. Clinical decisionmaking is particularly influenced by interpersonal relationships with colleagues, 39 patient conditions, availability of resources, 40 knowledge, and experience. 41 Of these, experience has been shown to enhance nurses’ abilities to make quick decisions 42 and fewer decision errors, 43 support the identification of salient cues, and foster the recognition and action on patterns of information. 44 , 45
Clinicians must develop the character and relational skills that enable them to perceive and understand their patient’s needs and concerns. This requires accurate interpretation of patient data that is relevant to the specific patient and situation. In nursing, this formation of moral agency focuses on learning to be responsible in particular ways demanded by the practice, and to pay attention and intelligently discern changes in patients’ concerns and/or clinical condition that require action on the part of the nurse or other health care workers to avert potential compromises to quality care.
Formation of the clinician’s character, skills, and habits are developed in schools and particular practice communities within a larger practice tradition. As Dunne notes,
A practice is not just a surface on which one can display instant virtuosity. It grounds one in a tradition that has been formed through an elaborate development and that exists at any juncture only in the dispositions (slowly and perhaps painfully acquired) of its recognized practitioners. The question may of course be asked whether there are any such practices in the contemporary world, whether the wholesale encroachment of Technique has not obliterated them—and whether this is not the whole point of MacIntyre’s recipe of withdrawal, as well as of the post-modern story of dispossession 11 (p. 378).
Clearly Dunne is engaging in critical reflection about the conditions for developing character, skills, and habits for skillful and ethical comportment of practitioners, as well as to act as moral agents for patients so that they and their families receive safe, effective, and compassionate care.
Professional socialization or professional values, while necessary, do not adequately address character and skill formation that transform the way the practitioner exists in his or her world, what the practitioner is capable of noticing and responding to, based upon well-established patterns of emotional responses, skills, dispositions to act, and the skills to respond, decide, and act. 46 The need for character and skill formation of the clinician is what makes a practice stand out from a mere technical, repetitious manufacturing process. 11 , 30 , 47
In nursing and medicine, many have questioned whether current health care institutions are designed to promote or hinder enlightened, compassionate practice, or whether they have deteriorated into commercial institutional models that focus primarily on efficiency and profit. MacIntyre points out the links between the ongoing development and improvement of practice traditions and the institutions that house them:
Lack of justice, lack of truthfulness, lack of courage, lack of the relevant intellectual virtues—these corrupt traditions, just as they do those institutions and practices which derive their life from the traditions of which they are the contemporary embodiments. To recognize this is of course also to recognize the existence of an additional virtue, one whose importance is perhaps most obvious when it is least present, the virtue of having an adequate sense of the traditions to which one belongs or which confront one. This virtue is not to be confused with any form of conservative antiquarianism; I am not praising those who choose the conventional conservative role of laudator temporis acti. It is rather the case that an adequate sense of tradition manifests itself in a grasp of those future possibilities which the past has made available to the present. Living traditions, just because they continue a not-yet-completed narrative, confront a future whose determinate and determinable character, so far as it possesses any, derives from the past 30 (p. 207).
It would be impossible to capture all the situated and distributed knowledge outside of actual practice situations and particular patients. Simulations are powerful as teaching tools to enable nurses’ ability to think critically because they give students the opportunity to practice in a simplified environment. However, students can be limited in their inability to convey underdetermined situations where much of the information is based on perceptions of many aspects of the patient and changes that have occurred over time. Simulations cannot have the sub-cultures formed in practice settings that set the social mood of trust, distrust, competency, limited resources, or other forms of situated possibilities.
One of the hallmark studies in nursing providing keen insight into understanding the influence of experience was a qualitative study of adult, pediatric, and neonatal intensive care unit (ICU) nurses, where the nurses were clustered into advanced beginner, intermediate, and expert level of practice categories. The advanced beginner (having up to 6 months of work experience) used procedures and protocols to determine which clinical actions were needed. When confronted with a complex patient situation, the advanced beginner felt their practice was unsafe because of a knowledge deficit or because of a knowledge application confusion. The transition from advanced beginners to competent practitioners began when they first had experience with actual clinical situations and could benefit from the knowledge gained from the mistakes of their colleagues. Competent nurses continuously questioned what they saw and heard, feeling an obligation to know more about clinical situations. In doing do, they moved from only using care plans and following the physicians’ orders to analyzing and interpreting patient situations. Beyond that, the proficient nurse acknowledged the changing relevance of clinical situations requiring action beyond what was planned or anticipated. The proficient nurse learned to acknowledge the changing needs of patient care and situation, and could organize interventions “by the situation as it unfolds rather than by preset goals 48 (p. 24). Both competent and proficient nurses (that is, intermediate level of practice) had at least two years of ICU experience. 48 Finally, the expert nurse had a more fully developed grasp of a clinical situation, a sense of confidence in what is known about the situation, and could differentiate the precise clinical problem in little time. 48
Expertise is acquired through professional experience and is indicative of a nurse who has moved beyond mere proficiency. As Gadamer 29 points out, experience involves a turning around of preconceived notions, preunderstandings, and extends or adds nuances to understanding. Dewey 49 notes that experience requires a prepared “creature” and an enriched environment. The opportunity to reflect and narrate one’s experiential learning can clarify, extend, or even refute experiential learning.
Experiential learning requires time and nurturing, but time alone does not ensure experiential learning. Aristotle linked experiential learning to the development of character and moral sensitivities of a person learning a practice. 50 New nurses/new graduates have limited work experience and must experience continuing learning until they have reached an acceptable level of performance. 51 After that, further improvements are not predictable, and years of experience are an inadequate predictor of expertise. 52
The most effective knower and developer of practical knowledge creates an ongoing dialogue and connection between lessons of the day and experiential learning over time. Gadamer, in a late life interview, highlighted the open-endedness and ongoing nature of experiential learning in the following interview response:
Being experienced does not mean that one now knows something once and for all and becomes rigid in this knowledge; rather, one becomes more open to new experiences. A person who is experienced is undogmatic. Experience has the effect of freeing one to be open to new experience … In our experience we bring nothing to a close; we are constantly learning new things from our experience … this I call the interminability of all experience 32 (p. 403).
Practical endeavor, supported by scientific knowledge, requires experiential learning, the development of skilled know-how, and perceptual acuity in order to make the scientific knowledge relevant to the situation. Clinical perceptual and skilled know-how helps the practitioner discern when particular scientific findings might be relevant. 53
Often experience and knowledge, confirmed by experimentation, are treated as oppositions, an either-or choice. However, in practice it is readily acknowledged that experiential knowledge fuels scientific investigation, and scientific investigation fuels further experiential learning. Experiential learning from particular clinical cases can help the clinician recognize future similar cases and fuel new scientific questions and study. For example, less experienced nurses—and it could be argued experienced as well—can use nursing diagnoses practice guidelines as part of their professional advancement. Guidelines are used to reflect their interpretation of patients’ needs, responses, and situation, 54 a process that requires critical thinking and decisionmaking. 55 , 56 Using guidelines also reflects one’s problem identification and problem-solving abilities. 56 Conversely, the ability to proficiently conduct a series of tasks without nursing diagnoses is the hallmark of expertise. 39 , 57
Experience precedes expertise. As expertise develops from experience and gaining knowledge and transitions to the proficiency stage, the nurses’ thinking moves from steps and procedures (i.e., task-oriented care) toward “chunks” or patterns 39 (i.e., patient-specific care). In doing so, the nurse thinks reflectively, rather than merely accepting statements and performing procedures without significant understanding and evaluation. 34 Expert nurses do not rely on rules and logical thought processes in problem-solving and decisionmaking. 39 Instead, they use abstract principles, can see the situation as a complex whole, perceive situations comprehensively, and can be fully involved in the situation. 48 Expert nurses can perform high-level care without conscious awareness of the knowledge they are using, 39 , 58 and they are able to provide that care with flexibility and speed. Through a combination of knowledge and skills gained from a range of theoretical and experiential sources, expert nurses also provide holistic care. 39 Thus, the best care comes from the combination of theoretical, tacit, and experiential knowledge. 59 , 60
Experts are thought to eventually develop the ability to intuitively know what to do and to quickly recognize critical aspects of the situation. 22 Some have proposed that expert nurses provide high-quality patient care, 61 , 62 but that is not consistently documented—particularly in consideration of patient outcomes—and a full understanding between the differential impact of care rendered by an “expert” nurse is not fully understood. In fact, several studies have found that length of professional experience is often unrelated and even negatively related to performance measures and outcomes. 63 , 64
In a review of the literature on expertise in nursing, Ericsson and colleagues 65 found that focusing on challenging, less-frequent situations would reveal individual performance differences on tasks that require speed and flexibility, such as that experienced during a code or an adverse event. Superior performance was associated with extensive training and immediate feedback about outcomes, which can be obtained through continual training, simulation, and processes such as root-cause analysis following an adverse event. Therefore, efforts to improve performance benefited from continual monitoring, planning, and retrospective evaluation. Even then, the nurse’s ability to perform as an expert is dependent upon their ability to use intuition or insights gained through interactions with patients. 39
Intuition and Perception
Intuition is the instant understanding of knowledge without evidence of sensible thought. 66 According to Young, 67 intuition in clinical practice is a process whereby the nurse recognizes something about a patient that is difficult to verbalize. Intuition is characterized by factual knowledge, “immediate possession of knowledge, and knowledge independent of the linear reasoning process” 68 (p. 23). When intuition is used, one filters information initially triggered by the imagination, leading to the integration of all knowledge and information to problem solve. 69 Clinicians use their interactions with patients and intuition, drawing on tacit or experiential knowledge, 70 , 71 to apply the correct knowledge to make the correct decisions to address patient needs. Yet there is a “conflated belief in the nurses’ ability to know what is best for the patient” 72 (p. 251) because the nurses’ and patients’ identification of the patients’ needs can vary. 73
A review of research and rhetoric involving intuition by King and Appleton 62 found that all nurses, including students, used intuition (i.e., gut feelings). They found evidence, predominately in critical care units, that intuition was triggered in response to knowledge and as a trigger for action and/or reflection with a direct bearing on the analytical process involved in patient care. The challenge for nurses was that rigid adherence to checklists, guidelines, and standardized documentation, 62 ignored the benefits of intuition. This view was furthered by Rew and Barrow 68 , 74 in their reviews of the literature, where they found that intuition was imperative to complex decisionmaking, 68 difficult to measure and assess in a quantitative manner, and was not linked to physiologic measures. 74
Intuition is a way of explaining professional expertise. 75 Expert nurses rely on their intuitive judgment that has been developed over time. 39 , 76 Intuition is an informal, nonanalytically based, unstructured, deliberate calculation that facilitates problem solving, 77 a process of arriving at salient conclusions based on relatively small amounts of knowledge and/or information. 78 Experts can have rapid insight into a situation by using intuition to recognize patterns and similarities, achieve commonsense understanding, and sense the salient information combined with deliberative rationality. 10 Intuitive recognition of similarities and commonalities between patients are often the first diagnostic clue or early warning, which must then be followed up with critical evaluation of evidence among the competing conditions. This situation calls for intuitive judgment that can distinguish “expert human judgment from the decisions” made by a novice 79 (p. 23).
Shaw 80 equates intuition with direct perception. Direct perception is dependent upon being able to detect complex patterns and relationships that one has learned through experience are important. Recognizing these patterns and relationships generally occurs rapidly and is complex, making it difficult to articulate or describe. Perceptual skills, like those of the expert nurse, are essential to recognizing current and changing clinical conditions. Perception requires attentiveness and the development of a sense of what is salient. Often in nursing and medicine, means and ends are fused, as is the case for a “good enough” birth experience and a peaceful death.
- Applying Practice Evidence
Research continues to find that using evidence-based guidelines in practice, informed through research evidence, improves patients’ outcomes. 81–83 Research-based guidelines are intended to provide guidance for specific areas of health care delivery. 84 The clinician—both the novice and expert—is expected to use the best available evidence for the most efficacious therapies and interventions in particular instances, to ensure the highest-quality care, especially when deviations from the evidence-based norm may heighten risks to patient safety. Otherwise, if nursing and medicine were exact sciences, or consisted only of techne, then a 1:1 relationship could be established between results of aggregated evidence-based research and the best path for all patients.
Evaluating Evidence
Before research should be used in practice, it must be evaluated. There are many complexities and nuances in evaluating the research evidence for clinical practice. Evaluation of research behind evidence-based medicine requires critical thinking and good clinical judgment. Sometimes the research findings are mixed or even conflicting. As such, the validity, reliability, and generalizability of available research are fundamental to evaluating whether evidence can be applied in practice. To do so, clinicians must select the best scientific evidence relevant to particular patients—a complex process that involves intuition to apply the evidence. Critical thinking is required for evaluating the best available scientific evidence for the treatment and care of a particular patient.
Good clinical judgment is required to select the most relevant research evidence. The best clinical judgment, that is, reasoning across time about the particular patient through changes in the patient’s concerns and condition and/or the clinician’s understanding, are also required. This type of judgment requires clinicians to make careful observations and evaluations of the patient over time, as well as know the patient’s concerns and social circumstances. To evolve to this level of judgment, additional education beyond clinical preparation if often required.
Sources of Evidence
Evidence that can be used in clinical practice has different sources and can be derived from research, patient’s preferences, and work-related experience. 85 , 86 Nurses have been found to obtain evidence from experienced colleagues believed to have clinical expertise and research-based knowledge 87 as well as other sources.
For many years now, randomized controlled trials (RCTs) have often been considered the best standard for evaluating clinical practice. Yet, unless the common threats to the validity (e.g., representativeness of the study population) and reliability (e.g., consistency in interventions and responses of study participants) of RCTs are addressed, the meaningfulness and generalizability of the study outcomes are very limited. Relevant patient populations may be excluded, such as women, children, minorities, the elderly, and patients with multiple chronic illnesses. The dropout rate of the trial may confound the results. And it is easier to get positive results published than it is to get negative results published. Thus, RCTs are generalizable (i.e., applicable) only to the population studied—which may not reflect the needs of the patient under the clinicians care. In instances such as these, clinicians need to also consider applied research using prospective or retrospective populations with case control to guide decisionmaking, yet this too requires critical thinking and good clinical judgment.
Another source of available evidence may come from the gold standard of aggregated systematic evaluation of clinical trial outcomes for the therapy and clinical condition in question, be generated by basic and clinical science relevant to the patient’s particular pathophysiology or care need situation, or stem from personal clinical experience. The clinician then takes all of the available evidence and considers the particular patient’s known clinical responses to past therapies, their clinical condition and history, the progression or stages of the patient’s illness and recovery, and available resources.
In clinical practice, the particular is examined in relation to the established generalizations of science. With readily available summaries of scientific evidence (e.g., systematic reviews and practice guidelines) available to nurses and physicians, one might wonder whether deep background understanding is still advantageous. Might it not be expendable, since it is likely to be out of date given the current scientific evidence? But this assumption is a false opposition and false choice because without a deep background understanding, the clinician does not know how to best find and evaluate scientific evidence for the particular case in hand. The clinician’s sense of salience in any given situation depends on past clinical experience and current scientific evidence.
Evidence-Based Practice
The concept of evidence-based practice is dependent upon synthesizing evidence from the variety of sources and applying it appropriately to the care needs of populations and individuals. This implies that evidence-based practice, indicative of expertise in practice, appropriately applies evidence to the specific situations and unique needs of patients. 88 , 89 Unfortunately, even though providing evidence-based care is an essential component of health care quality, it is well known that evidence-based practices are not used consistently.
Conceptually, evidence used in practice advances clinical knowledge, and that knowledge supports independent clinical decisions in the best interest of the patient. 90 , 91 Decisions must prudently consider the factors not necessarily addressed in the guideline, such as the patient’s lifestyle, drug sensitivities and allergies, and comorbidities. Nurses who want to improve the quality and safety of care can do so though improving the consistency of data and information interpretation inherent in evidence-based practice.
Initially, before evidence-based practice can begin, there needs to be an accurate clinical judgment of patient responses and needs. In the course of providing care, with careful consideration of patient safety and quality care, clinicians must give attention to the patient’s condition, their responses to health care interventions, and potential adverse reactions or events that could harm the patient. Nonetheless, there is wide variation in the ability of nurses to accurately interpret patient responses 92 and their risks. 93 Even though variance in interpretation is expected, nurses are obligated to continually improve their skills to ensure that patients receive quality care safely. 94 Patients are vulnerable to the actions and experience of their clinicians, which are inextricably linked to the quality of care patients have access to and subsequently receive.
The judgment of the patient’s condition determines subsequent interventions and patient outcomes. Attaining accurate and consistent interpretations of patient data and information is difficult because each piece can have different meanings, and interpretations are influenced by previous experiences. 95 Nurses use knowledge from clinical experience 96 , 97 and—although infrequently—research. 98–100
Once a problem has been identified, using a process that utilizes critical thinking to recognize the problem, the clinician then searches for and evaluates the research evidence 101 and evaluates potential discrepancies. The process of using evidence in practice involves “a problem-solving approach that incorporates the best available scientific evidence, clinicians’ expertise, and patient’s preferences and values” 102 (p. 28). Yet many nurses do not perceive that they have the education, tools, or resources to use evidence appropriately in practice. 103
Reported barriers to using research in practice have included difficulty in understanding the applicability and the complexity of research findings, failure of researchers to put findings into the clinical context, lack of skills in how to use research in practice, 104 , 105 amount of time required to access information and determine practice implications, 105–107 lack of organizational support to make changes and/or use in practice, 104 , 97 , 105 , 107 and lack of confidence in one’s ability to critically evaluate clinical evidence. 108
When Evidence Is Missing
In many clinical situations, there may be no clear guidelines and few or even no relevant clinical trials to guide decisionmaking. In these cases, the latest basic science about cellular and genomic functioning may be the most relevant science, or by default, guestimation. Consequently, good patient care requires more than a straightforward, unequivocal application of scientific evidence. The clinician must be able to draw on a good understanding of basic sciences, as well as guidelines derived from aggregated data and information from research investigations.
Practical knowledge is shaped by one’s practice discipline and the science and technology relevant to the situation at hand. But scientific, formal, discipline-specific knowledge are not sufficient for good clinical practice, whether the discipline be law, medicine, nursing, teaching, or social work. Practitioners still have to learn how to discern generalizable scientific knowledge, know how to use scientific knowledge in practical situations, discern what scientific evidence/knowledge is relevant, assess how the particular patient’s situation differs from the general scientific understanding, and recognize the complexity of care delivery—a process that is complex, ongoing, and changing, as new evidence can overturn old.
Practice communities like individual practitioners may also be mistaken, as is illustrated by variability in practice styles and practice outcomes across hospitals and regions in the United States. This variability in practice is why practitioners must learn to critically evaluate their practice and continually improve their practice over time. The goal is to create a living self-improving tradition.
Within health care, students, scientists, and practitioners are challenged to learn and use different modes of thinking when they are conflated under one term or rubric, using the best-suited thinking strategies for taking into consideration the purposes and the ends of the reasoning. Learning to be an effective, safe nurse or physician requires not only technical expertise, but also the ability to form helping relationships and engage in practical ethical and clinical reasoning. 50 Good ethical comportment requires that both the clinician and the scientist take into account the notions of good inherent in clinical and scientific practices. The notions of good clinical practice must include the relevant significance and the human concerns involved in decisionmaking in particular situations, centered on clinical grasp and clinical forethought.
The Three Apprenticeships of Professional Education
We have much to learn in comparing the pedagogies of formation across the professions, such as is being done currently by the Carnegie Foundation for the Advancement of Teaching. The Carnegie Foundation’s broad research program on the educational preparation of the profession focuses on three essential apprenticeships:
To capture the full range of crucial dimensions in professional education, we developed the idea of a three-fold apprenticeship: (1) intellectual training to learn the academic knowledge base and the capacity to think in ways important to the profession; (2) a skill-based apprenticeship of practice; and (3) an apprenticeship to the ethical standards, social roles, and responsibilities of the profession, through which the novice is introduced to the meaning of an integrated practice of all dimensions of the profession, grounded in the profession’s fundamental purposes. 109
This framework has allowed the investigators to describe tensions and shortfalls as well as strengths of widespread teaching practices, especially at articulation points among these dimensions of professional training.
Research has demonstrated that these three apprenticeships are taught best when they are integrated so that the intellectual training includes skilled know-how, clinical judgment, and ethical comportment. In the study of nursing, exemplary classroom and clinical teachers were found who do integrate the three apprenticeships in all of their teaching, as exemplified by the following anonymous student’s comments:
With that as well, I enjoyed the class just because I do have clinical experience in my background and I enjoyed it because it took those practical applications and the knowledge from pathophysiology and pharmacology, and all the other classes, and it tied it into the actual aspects of like what is going to happen at work. For example, I work in the emergency room and question: Why am I doing this procedure for this particular patient? Beforehand, when I was just a tech and I wasn’t going to school, I’d be doing it because I was told to be doing it—or I’d be doing CPR because, you know, the doc said, start CPR. I really enjoy the Care and Illness because now I know the process, the pathophysiological process of why I’m doing it and the clinical reasons of why they’re making the decisions, and the prioritization that goes on behind it. I think that’s the biggest point. Clinical experience is good, but not everybody has it. Yet when these students transition from school and clinicals to their job as a nurse, they will understand what’s going on and why.
The three apprenticeships are equally relevant and intertwined. In the Carnegie National Study of Nursing Education and the companion study on medical education as well as in cross-professional comparisons, teaching that gives an integrated access to professional practice is being examined. Once the three apprenticeships are separated, it is difficult to reintegrate them. The investigators are encouraged by teaching strategies that integrate the latest scientific knowledge and relevant clinical evidence with clinical reasoning about particular patients in unfolding rather than static cases, while keeping the patient and family experience and concerns relevant to clinical concerns and reasoning.
Clinical judgment or phronesis is required to evaluate and integrate techne and scientific evidence.
Within nursing, professional practice is wise and effective usually to the extent that the professional creates relational and communication contexts where clients/patients can be open and trusting. Effectiveness depends upon mutual influence between patient and practitioner, student and learner. This is another way in which clinical knowledge is dialogical and socially distributed. The following articulation of practical reasoning in nursing illustrates the social, dialogical nature of clinical reasoning and addresses the centrality of perception and understanding to good clinical reasoning, judgment and intervention.
Clinical Grasp *
Clinical grasp describes clinical inquiry in action. Clinical grasp begins with perception and includes problem identification and clinical judgment across time about the particular transitions of particular patients. Garrett Chan 20 described the clinician’s attempt at finding an “optimal grasp” or vantage point of understanding. Four aspects of clinical grasp, which are described in the following paragraphs, include (1) making qualitative distinctions, (2) engaging in detective work, (3) recognizing changing relevance, and (4) developing clinical knowledge in specific patient populations.
Making Qualitative Distinctions
Qualitative distinctions refer to those distinctions that can be made only in a particular contextual or historical situation. The context and sequence of events are essential for making qualitative distinctions; therefore, the clinician must pay attention to transitions in the situation and judgment. Many qualitative distinctions can be made only by observing differences through touch, sound, or sight, such as the qualities of a wound, skin turgor, color, capillary refill, or the engagement and energy level of the patient. Another example is assessing whether the patient was more fatigued after ambulating to the bathroom or from lack of sleep. Likewise the quality of the clinician’s touch is distinct as in offering reassurance, putting pressure on a bleeding wound, and so on. 110
Engaging in Detective Work, Modus Operandi Thinking, and Clinical Puzzle Solving
Clinical situations are open ended and underdetermined. Modus operandi thinking keeps track of the particular patient, the way the illness unfolds, the meanings of the patient’s responses as they have occurred in the particular time sequence. Modus operandi thinking requires keeping track of what has been tried and what has or has not worked with the patient. In this kind of reasoning-in-transition, gains and losses of understanding are noticed and adjustments in the problem approach are made.
We found that teachers in a medical surgical unit at the University of Washington deliberately teach their students to engage in “detective work.” Students are given the daily clinical assignment of “sleuthing” for undetected drug incompatibilities, questionable drug dosages, and unnoticed signs and symptoms. For example, one student noted that an unusual dosage of a heart medication was being given to a patient who did not have heart disease. The student first asked her teacher about the unusually high dosage. The teacher, in turn, asked the student whether she had asked the nurse or the patient about the dosage. Upon the student’s questioning, the nurse did not know why the patient was receiving the high dosage and assumed the drug was for heart disease. The patient’s staff nurse had not questioned the order. When the student asked the patient, the student found that the medication was being given for tremors and that the patient and the doctor had titrated the dosage for control of the tremors. This deliberate approach to teaching detective work, or modus operandi thinking, has characteristics of “critical reflection,” but stays situated and engaged, ferreting out the immediate history and unfolding of events.
Recognizing Changing Clinical Relevance
The meanings of signs and symptoms are changed by sequencing and history. The patient’s mental status, color, or pain level may continue to deteriorate or get better. The direction, implication, and consequences for the changes alter the relevance of the particular facts in the situation. The changing relevance entailed in a patient transitioning from primarily curative care to primarily palliative care is a dramatic example, where symptoms literally take on new meanings and require new treatments.
Developing Clinical Knowledge in Specific Patient Populations
Extensive experience with a specific patient population or patients with particular injuries or diseases allows the clinician to develop comparisons, distinctions, and nuanced differences within the population. The comparisons between many specific patients create a matrix of comparisons for clinicians, as well as a tacit, background set of expectations that create population- and patient-specific detective work if a patient does not meet the usual, predictable transitions in recovery. What is in the background and foreground of the clinician’s attention shifts as predictable changes in the patient’s condition occurs, such as is seen in recovering from heart surgery or progressing through the predictable stages of labor and delivery. Over time, the clinician develops a deep background understanding that allows for expert diagnostic and interventions skills.
Clinical Forethought
Clinical forethought is intertwined with clinical grasp, but it is much more deliberate and even routinized than clinical grasp. Clinical forethought is a pervasive habit of thought and action in nursing practice, and also in medicine, as clinicians think about disease and recovery trajectories and the implications of these changes for treatment. Clinical forethought plays a role in clinical grasp because it structures the practical logic of clinicians. At least four habits of thought and action are evident in what we are calling clinical forethought: (1) future think, (2) clinical forethought about specific patient populations, (3) anticipation of risks for particular patients, and (4) seeing the unexpected.
Future think
Future think is the broadest category of this logic of practice. Anticipating likely immediate futures helps the clinician make good plans and decisions about preparing the environment so that responding rapidly to changes in the patient is possible. Without a sense of salience about anticipated signs and symptoms and preparing the environment, essential clinical judgments and timely interventions would be impossible in the typically fast pace of acute and intensive patient care. Future think governs the style and content of the nurse’s attentiveness to the patient. Whether in a fast-paced care environment or a slower-paced rehabilitation setting, thinking and acting with anticipated futures guide clinical thinking and judgment. Future think captures the way judgment is suspended in a predictive net of anticipation and preparing oneself and the environment for a range of potential events.
Clinical forethought about specific diagnoses and injuries
This habit of thought and action is so second nature to the experienced nurse that the new or inexperienced nurse may have difficulty finding out about what seems to other colleagues as “obvious” preparation for particular patients and situations. Clinical forethought involves much local specific knowledge about who is a good resource and how to marshal support services and equipment for particular patients.
Examples of preparing for specific patient populations are pervasive, such as anticipating the need for a pacemaker during surgery and having the equipment assembled ready for use to save essential time. Another example includes forecasting an accident victim’s potential injuries, and recognizing that intubation might be needed.

Anticipation of crises, risks, and vulnerabilities for particular patients
This aspect of clinical forethought is central to knowing the particular patient, family, or community. Nurses situate the patient’s problems almost like a topography of possibilities. This vital clinical knowledge needs to be communicated to other caregivers and across care borders. Clinical teaching could be improved by enriching curricula with narrative examples from actual practice, and by helping students recognize commonly occurring clinical situations in the simulation and clinical setting. For example, if a patient is hemodynamically unstable, then managing life-sustaining physiologic functions will be a main orienting goal. If the patient is agitated and uncomfortable, then attending to comfort needs in relation to hemodynamics will be a priority. Providing comfort measures turns out to be a central background practice for making clinical judgments and contains within it much judgment and experiential learning.
When clinical teaching is too removed from typical contingencies and strong clinical situations in practice, students will lack practice in active thinking-in-action in ambiguous clinical situations. In the following example, an anonymous student recounted her experiences of meeting a patient:
I was used to different equipment and didn’t know how things went, didn’t know their routine, really. You can explain all you want in class, this is how it’s going to be, but when you get there … . Kim was my first instructor and my patient that she assigned me to—I walked into the room and he had every tube imaginable. And so I was a little overwhelmed. It’s not necessarily even that he was that critical … . She asked what tubes here have you seen? Well, I know peripheral lines. You taught me PICC [peripherally inserted central catheter] lines, and we just had that, but I don’t really feel comfortable doing it by myself, without you watching to make sure that I’m flushing it right and how to assess it. He had a chest tube and I had seen chest tubes, but never really knew the depth of what you had to assess and how you make sure that it’s all kosher and whatever. So she went through the chest tube and explained, it’s just bubbling a little bit and that’s okay. The site, check the site. The site looked okay and that she’d say if it wasn’t okay, this is what it might look like … . He had a feeding tube. I had done feeding tubes but that was like a long time ago in my LPN experiences schooling. So I hadn’t really done too much with the feeding stuff either … . He had a [nasogastric] tube, and knew pretty much about that and I think at the time it was clamped. So there were no issues with the suction or whatever. He had a Foley catheter. He had a feeding tube, a chest tube. I can’t even remember but there were a lot.
As noted earlier, a central characteristic of a practice discipline is that a self-improving practice requires ongoing experiential learning. One way nurse educators can enhance clinical inquiry is by increasing pedagogies of experiential learning. Current pedagogies for experiential learning in nursing include extensive preclinical study, care planning, and shared postclinical debriefings where students share their experiential learning with their classmates. Experiential learning requires open learning climates where students can discuss and examine transitions in understanding, including their false starts, or their misconceptions in actual clinical situations. Nursing educators typically develop open and interactive clinical learning communities, so that students seem committed to helping their classmates learn from their experiences that may have been difficult or even unsafe. One anonymous nurse educator described how students extend their experiential learning to their classmates during a postclinical conference:
So for example, the patient had difficulty breathing and the student wanted to give the meds instead of addressing the difficulty of breathing. Well, while we were sharing information about their patients, what they did that day, I didn’t tell the student to say this, but she said, ‘I just want to tell you what I did today in clinical so you don’t do the same thing, and here’s what happened.’ Everybody’s listening very attentively and they were asking her some questions. But she shared that. She didn’t have to. I didn’t tell her, you must share that in postconference or anything like that, but she just went ahead and shared that, I guess, to reinforce what she had learned that day but also to benefit her fellow students in case that thing comes up with them.
The teacher’s response to this student’s honesty and generosity exemplifies her own approach to developing an open community of learning. Focusing only on performance and on “being correct” prevents learning from breakdown or error and can dampen students’ curiosity and courage to learn experientially.
Seeing the unexpected
One of the keys to becoming an expert practitioner lies in how the person holds past experiential learning and background habitual skills and practices. This is a skill of foregrounding attention accurately and effectively in response to the nature of situational demands. Bourdieu 29 calls the recognition of the situation central to practical reasoning. If nothing is routinized as a habitual response pattern, then practitioners will not function effectively in emergencies. Unexpected occurrences may be overlooked. However, if expectations are held rigidly, then subtle changes from the usual will be missed, and habitual, rote responses will inappropriately rule. The clinician must be flexible in shifting between what is in background and foreground. This is accomplished by staying curious and open. The clinical “certainty” associated with perceptual grasp is distinct from the kind of “certainty” achievable in scientific experiments and through measurements. Recognition of similar or paradigmatic clinical situations is similar to “face recognition” or recognition of “family resemblances.” This concept is subject to faulty memory, false associative memories, and mistaken identities; therefore, such perceptual grasp is the beginning of curiosity and inquiry and not the end. Assessment and validation are required. In rapidly moving clinical situations, perceptual grasp is the starting point for clarification, confirmation, and action. Having the clinician say out loud how he or she is understanding the situation gives an opportunity for confirmation and disconfirmation from other clinicians present. 111 The relationship between foreground and background of attention needs to be fluid, so that missed expectations allow the nurse to see the unexpected. For example, when the background rhythm of a cardiac monitor changes, the nurse notices, and what had been background tacit awareness becomes the foreground of attention. A hallmark of expertise is the ability to notice the unexpected. 20 Background expectations of usual patient trajectories form with experience. Tacit expectations for patient trajectories form that enable the nurse to notice subtle failed expectations and pay attention to early signs of unexpected changes in the patient's condition. Clinical expectations gained from caring for similar patient populations form a tacit clinical forethought that enable the experienced clinician to notice missed expectations. Alterations from implicit or explicit expectations set the stage for experiential learning, depending on the openness of the learner.
Learning to provide safe and quality health care requires technical expertise, the ability to think critically, experience, and clinical judgment. The high-performance expectation of nurses is dependent upon the nurses’ continual learning, professional accountability, independent and interdependent decisionmaking, and creative problem-solving abilities.
This section of the paper was condensed and paraphrased from Benner, Hooper-Kyriakidis, and Stannard. 23 Patricia Hooper-Kyriakidis wrote the section on clinical grasp, and Patricia Benner wrote the section on clinical forethought.
- Cite this Page Benner P, Hughes RG, Sutphen M. Clinical Reasoning, Decisionmaking, and Action: Thinking Critically and Clinically. In: Hughes RG, editor. Patient Safety and Quality: An Evidence-Based Handbook for Nurses. Rockville (MD): Agency for Healthcare Research and Quality (US); 2008 Apr. Chapter 6.
- PDF version of this page (147K)
In this Page
- Clinical Grasp
Other titles in this collection
- Advances in Patient Safety
Related information
- PMC PubMed Central citations
- PubMed Links to PubMed
Similar articles in PubMed
- Nurses' reasoning process during care planning taking pressure ulcer prevention as an example. A think-aloud study. [Int J Nurs Stud. 2007] Nurses' reasoning process during care planning taking pressure ulcer prevention as an example. A think-aloud study. Funkesson KH, Anbäcken EM, Ek AC. Int J Nurs Stud. 2007 Sep; 44(7):1109-19. Epub 2006 Jun 27.
- Registered nurses' clinical reasoning skills and reasoning process: A think-aloud study. [Nurse Educ Today. 2016] Registered nurses' clinical reasoning skills and reasoning process: A think-aloud study. Lee J, Lee YJ, Bae J, Seo M. Nurse Educ Today. 2016 Nov; 46:75-80. Epub 2016 Aug 15.
- Combining the arts: an applied critical thinking approach in the skills laboratory. [Nursingconnections. 2000] Combining the arts: an applied critical thinking approach in the skills laboratory. Peterson MJ, Bechtel GA. Nursingconnections. 2000 Summer; 13(2):43-9.
- Review About critical thinking. [Dynamics. 2004] Review About critical thinking. Hynes P, Bennett J. Dynamics. 2004 Fall; 15(3):26-9.
- Review The 'five rights' of clinical reasoning: an educational model to enhance nursing students' ability to identify and manage clinically 'at risk' patients. [Nurse Educ Today. 2010] Review The 'five rights' of clinical reasoning: an educational model to enhance nursing students' ability to identify and manage clinically 'at risk' patients. Levett-Jones T, Hoffman K, Dempsey J, Jeong SY, Noble D, Norton CA, Roche J, Hickey N. Nurse Educ Today. 2010 Aug; 30(6):515-20. Epub 2009 Nov 30.
Recent Activity
- Clinical Reasoning, Decisionmaking, and Action: Thinking Critically and Clinical... Clinical Reasoning, Decisionmaking, and Action: Thinking Critically and Clinically - Patient Safety and Quality
Your browsing activity is empty.
Activity recording is turned off.
Turn recording back on
Connect with NLM
National Library of Medicine 8600 Rockville Pike Bethesda, MD 20894
Web Policies FOIA HHS Vulnerability Disclosure
Help Accessibility Careers
Critical Thinking in Nursing
- First Online: 02 January 2023
Cite this chapter

- Şefika Dilek Güven 3
Part of the book series: Integrated Science ((IS,volume 12))
1268 Accesses
Critical thinking is an integral part of nursing, especially in terms of professionalization and independent clinical decision-making. It is necessary to think critically to provide adequate, creative, and effective nursing care when making the right decisions for practices and care in the clinical setting and solving various ethical issues encountered. Nurses should develop their critical thinking skills so that they can analyze the problems of the current century, keep up with new developments and changes, cope with nursing problems they encounter, identify more complex patient care needs, provide more systematic care, give the most appropriate patient care in line with the education they have received, and make clinical decisions. The present chapter briefly examines critical thinking, how it relates to nursing, and which skills nurses need to develop as critical thinkers.
Graphical Abstract/Art Performance

Critical thinking in nursing.
This painting shows a nurse and how she is thinking critically. On the right side are the stages of critical thinking and on the left side, there are challenges that a nurse might face. The entire background is also painted in several colors to represent a kind of intellectual puzzle. It is made using colored pencils and markers.
(Adapted with permission from the Association of Science and Art (ASA), Universal Scientific Education and Research Network (USERN); Painting by Mahshad Naserpour).
Unless the individuals of a nation thinkers, the masses can be drawn in any direction. Mustafa Kemal Atatürk
This is a preview of subscription content, log in via an institution to check access.
Access this chapter
Subscribe and save.
- Get 10 units per month
- Download Article/Chapter or eBook
- 1 Unit = 1 Article or 1 Chapter
- Cancel anytime
- Available as PDF
- Read on any device
- Instant download
- Own it forever
- Available as EPUB and PDF
- Compact, lightweight edition
- Dispatched in 3 to 5 business days
- Free shipping worldwide - see info
- Durable hardcover edition
Tax calculation will be finalised at checkout
Purchases are for personal use only
Institutional subscriptions
Similar content being viewed by others

Thinking Critically About the Quality of Critical Thinking Definitions and Measures

Criticality in Osteopathic Medicine: Exploring the Relationship between Critical Thinking and Clinical Reasoning

A guide to critical thinking: implications for dental education
Bilgiç Ş, Kurtuluş Tosun Z (2016) Birinci ve son sınıf hemşirelik öğrencilerinde eleştirel düşünme ve etkileyen faktörler. Sağlık Bilimleri ve Meslekleri Dergisi 3(1):39–47
Article Google Scholar
Kantek F, Yıldırım N (2019) The effects of nursing education on critical thinking of students: a meta-analysis. Florence Nightingale Hemşirelik Dergisi 27(1):17–25
Ennis R (1996) Critical thinking dispositions: their nature and assessability. Informal Logic 18(2):165–182
Riddell T (2007) Critical assumptions: thinking critically about critical thinking. J Nurs Educ 46(3):121–126
Cüceloğlu D (2001) İyi düşün doğru karar ver. Remzi Kitabevi, pp 242–284
Google Scholar
Kurnaz A (2019) Eleştirel düşünme öğretimi etkinlikleri Planlama-Uygulama ve Değerlendirme. Eğitim yayın evi, p 27
Doğanay A, Ünal F (2006) Eleştirel düşünmenin öğretimi. In: İçerik Türlerine Dayalı Öğretim. Ankara Nobel Yayınevi, pp 209–261
Scheffer B-K, Rubenfeld M-G (2000) A consensus statement on critical thinking in nursing. J Nurs Educ 39(8):352–359
Article CAS Google Scholar
Rubenfeld M-G, Scheffer B (2014) Critical thinking tactics for nurses. Jones & Bartlett Publishers, pp 5–6, 7, 19–20
Gobet F (2005) Chunking models of expertise: implications for education. Appl Cogn Psychol 19:183–204
Ay F-A (2008) Mesleki temel kavramlar. In: Temel hemşirelik: Kavramlar, ilkeler, uygulamalar. İstanbul Medikal Yayıncılık, pp 205–220
Birol L (2010) Hemşirelik bakımında sistematik yaklaşım. In: Hemşirelik süreci. Berke Ofset Matbaacılık, pp 35–45
Twibell R, Ryan M, Hermiz M (2005) Faculty perceptions of critical thinking in student clinical experiences. J Nurs Educ 44(2):71–79
The Importance of Critical Thinking in Nursing. 19 November 2018 by Carson-Newman University Online. https://onlinenursing.cn.edu/news/value-critical-thinking-nursing
Suzanne C, Smeltzer Brenda G, Bare Janice L, Cheever HK (2010) Definition of critical thinking, critical thinking process. Medical surgical nursing. Lippincott, Williams & Wilkins, pp 27–28
Profetto-McGrath J (2003) The relationship of critical thinking skills and critical thinking dispositions of baccalaureate nursing students. J Adv Nurs 43(6):569–577
Elaine S, Mary C (2002) Critical thinking in nursing education: literature review. Int J Nurs Pract 8(2):89–98
Brunt B-A (2005) Critical thinking in nursing: an integrated review. J Continuing Educ Nurs 36(2):60–67
Carter L-M, Rukholm E (2008) A study of critical thinking, teacher–student interaction, and discipline-specific writing in an online educational setting for registered nurses. J Continuing Educ Nurs 39(3):133–138
Daly W-M (2001) The development of an alternative method in the assessment of critical thinking as an outcome of nursing education. J Adv Nurs 36(1):120–130
Edwards S-L (2007) Critical thinking: a two-phase framework. Nurse Educ Pract 7(5):303–314
Rogal S-M, Young J (2008) Exploring critical thinking in critical care nursing education: a pilot study. J Continuing Educ Nurs 39(1):28–33
Worrell J-A, Profetto-McGrath J (2007) Critical thinking as an outcome of context-based learning among post RN students: a literature review. Nurse Educ Today 27(5):420–426
Morrall P, Goodman B (2013) Critical thinking, nurse education and universities: some thoughts on current issues and implications for nursing practice. Nurse Educ Today 33(9):935–937
Raymond-Seniuk C, Profetto-McGrath J (2011) Can one learn to think critically?—a philosophical exploration. Open Nurs J 5:45–51
Download references
Author information
Authors and affiliations.
Nevşehir Hacı Bektaş Veli University, Semra ve Vefa Küçük, Faculty of Health Sciences, Nursing Department, 2000 Evler Mah. Damat İbrahim Paşa Yerleşkesi, Nevşehir, Turkey
Şefika Dilek Güven
You can also search for this author in PubMed Google Scholar
Corresponding author
Correspondence to Şefika Dilek Güven .
Editor information
Editors and affiliations.
Universal Scientific Education and Research Network (USERN), Stockholm, Sweden
Nima Rezaei
Rights and permissions
Reprints and permissions
Copyright information
© 2023 The Author(s), under exclusive license to Springer Nature Switzerland AG
About this chapter
Güven, Ş.D. (2023). Critical Thinking in Nursing. In: Rezaei, N. (eds) Brain, Decision Making and Mental Health. Integrated Science, vol 12. Springer, Cham. https://doi.org/10.1007/978-3-031-15959-6_10
Download citation
DOI : https://doi.org/10.1007/978-3-031-15959-6_10
Published : 02 January 2023
Publisher Name : Springer, Cham
Print ISBN : 978-3-031-15958-9
Online ISBN : 978-3-031-15959-6
eBook Packages : Behavioral Science and Psychology Behavioral Science and Psychology (R0)
Share this chapter
Anyone you share the following link with will be able to read this content:
Sorry, a shareable link is not currently available for this article.
Provided by the Springer Nature SharedIt content-sharing initiative
- Publish with us
Policies and ethics
- Find a journal
- Track your research
The Nursing Process: A Comprehensive Guide

In 1958, Ida Jean Orlando began developing the nursing process still evident in nursing care today. According to Orlando’s theory, the patient’s behavior sets the nursing process in motion. Through the nurse ‘s knowledge to analyze and diagnose the behavior to determine the patient’s needs.
Application of the fundamental principles of critical thinking , client-centered approaches to treatment, goal-oriented tasks, evidence-based practice (EBP) recommendations, and nursing intuition, the nursing process functions as a systematic guide to client-centered care with five subsequent steps. These are assessment , diagnosis, planning, implementation, and evaluation ( ADPIE ).
Table of Contents
What is the nursing process.
- What is the purpose of the nursing process?
Characteristics of the nursing process
Nursing process steps, collecting data, objective data or signs, subjective data or symptoms, verbal data, nonverbal data, primary source, secondary source, tertiary source, health interview, physical examination, observation, validating data, documenting data.
- 2. Diagnosis: “What is the problem?”
Initial Planning
Ongoing planning, discharge planning, developing a nursing care plan, behavioral nursing interventions, community nursing interventions, family nursing interventions, health system nursing interventions, physiological nursing interventions, safety nursing interventions, skills used in implementing nursing care, 1. reassessing the client, 2. determining the nurse’s need for assistance, nursing intervention categories, independent nursing interventions, dependent nursing interventions, interdependent nursing interventions, 4. supervising the delegated care, 5. documenting nursing activities, 1. collecting data, 2. comparing data with desired outcomes, 3. analyzing client’s response relating to nursing activities, 4. identifying factors contributing to success or failure, 5. continuing, modifying, or terminating the nursing care plan, 6. discharge planning.
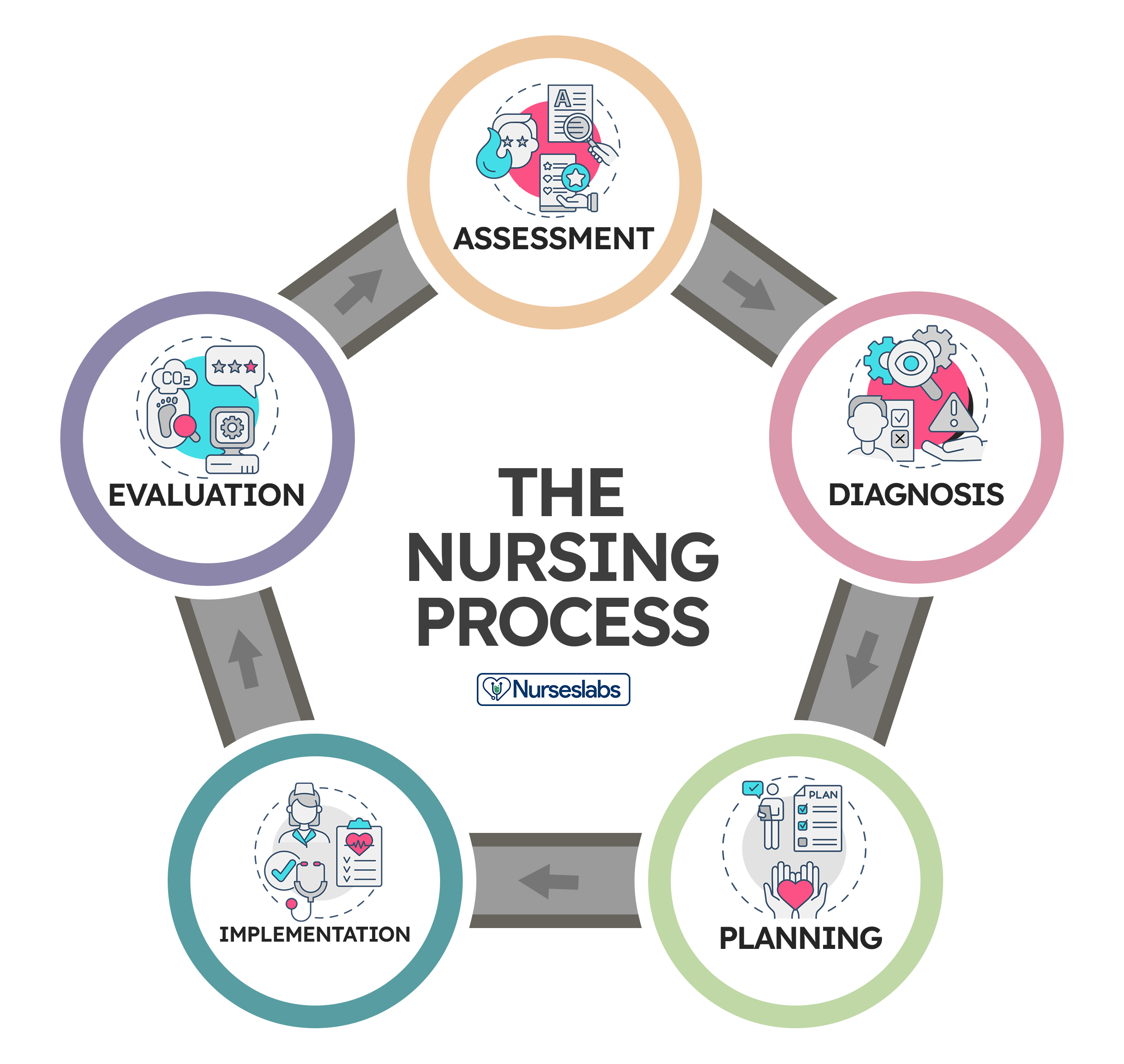
The nursing process is defined as a systematic, rational method of planning that guides all nursing actions in delivering holistic and patient-focused care. The nursing process is a form of scientific reasoning and requires the nurse’s critical thinking to provide the best care possible to the client.
What is the purpose of the nursing process?
The following are the purposes of the nursing process:
- To identify the client’s health status and actual or potential health care problems or needs (through assessment).
- To establish plans to meet the identified needs.
- To deliver specific nursing interventions to meet those needs.
- To apply the best available caregiving evidence and promote human functions and responses to health and illness (ANA, 2010).
- To protect nurses against legal problems related to nursing care when the standards of the nursing process are followed correctly.
- To help the nurse perform in a systematically organized way their practice.
- To establish a database about the client’s health status, health concerns, response to illness, and the ability to manage health care needs.
The following are the unique characteristics of the nursing process:
- Patient-centered . The unique approach of the nursing process requires care respectful of and responsive to the individual patient’s needs, preferences, and values. The nurse functions as a patient advocate by keeping the patient’s right to practice informed decision-making and maintaining patient-centered engagement in the health care setting.
- Interpersonal . The nursing process provides the basis for the therapeutic process in which the nurse and patient respect each other as individuals, both of them learning and growing due to the interaction. It involves the interaction between the nurse and the patient with a common goal.
- Collaborative . The nursing process functions effectively in nursing and inter-professional teams, promoting open communication, mutual respect, and shared decision-making to achieve quality patient care .
- Dynamic and cyclical .The nursing process is a dynamic, cyclical process in which each phase interacts with and is influenced by the other phases.
- Requires critical thinking . The use of the nursing process requires critical thinking which is a vital skill required for nurses in identifying client problems and implementing interventions to promote effective care outcomes.
The nursing process consists of five steps: assessment, diagnosis, planning, implementation, and evaluation . The acronym ADPIE is an easy way to remember the components of the nursing process. Nurses need to learn how to apply the process step-by-step. However, as critical thinking develops through experience, they learn how to move back and forth among the steps of the nursing process.
The steps of the nursing process are not separate entities but overlapping, continuing subprocesses. Apart from understanding nursing diagnoses and their definitions, the nurse promotes awareness of defining characteristics and behaviors of the diagnoses, related factors to the selected nursing diagnoses, and the interventions suited for treating the diagnoses.
The steps of the nursing process are detailed below:
1. Assessment: “What data is collected?”
The first phase of the nursing process is assessment . It involves collecting, organizing, validating, and documenting the clients’ health status. This data can be obtained in a variety of ways. Usually, when the nurse first encounters a patient, the nurse is expected to assess to identify the patient’s health problems as well as the physiological, psychological, and emotional state and to establish a database about the client’s response to health concerns or illness and the ability to manage health care needs. Critical thinking skills are essential to the assessment, thus requiring concept-based curriculum changes.
Data collection is the process of gathering information regarding a client’s health status. The process must be systematic and continuous in collecting data to prevent the omission of important information concerning the client.
The best way to collect data is through head-to-toe assessment. Learn more about it at our guide: Head to Toe Assessment: Complete Physical Assessment Guide
Types of Data
Data collected about a client generally falls into objective or subjective categories, but data can also be verbal and nonverbal.
Objective data are overt, measurable, tangible data collected via the senses, such as sight, touch , smell , or hearing , and compared to an accepted standard, such as vital signs, intake and output , height and weight, body temperature, pulse, and respiratory rates, blood pressure , vomiting , distended abdomen, presence of edema , lung sounds, crying, skin color, and presence of diaphoresis.
Subjective data involve covert information, such as feelings, perceptions, thoughts, sensations, or concerns that are shared by the patient and can be verified only by the patient, such as nausea , pain , numbness, pruritus, attitudes, beliefs, values, and perceptions of the health concern and life events.
Verbal data are spoken or written data such as statements made by the client or by a secondary source. Verbal data requires the listening skills of the nurse to assess difficulties such as slurring, tone of voice, assertiveness, anxiety , difficulty in finding the desired word, and flight of ideas.
Nonverbal data are observable behavior transmitting a message without words, such as the patient’s body language, general appearance , facial expressions, gestures, eye contact, proxemics (distance), body language, touch, posture, clothing. Nonverbal data obtained can sometimes be more powerful than verbal data, as the client’s body language may not be congruent with what they really think or feel. Obtaining and analyzing nonverbal data can help reinforce other forms of data and understand what the patient really feels.
Sources of Data
Sources of data can be primary, secondary, and tertiary . The client is the primary source of data, while family members , support persons, records and reports, other health professionals, laboratory and diagnostics fall under secondary sources.
The client is the only primary source of data and the only one who can provide subjective data. Anything the client says or reports to the members of the healthcare team is considered primary.
A source is considered secondary data if it is provided from someone else other than the client but within the client’s frame of reference. Information provided by the client’s family or significant others are considered secondary sources of data if the client cannot speak for themselves, is lacking facts and understanding, or is a child. Additionally, the client’s records and assessment data from other nurses or other members of the healthcare team are considered secondary sources of data.
Sources from outside the client’s frame of reference are considered tertiary sources of data . Examples of tertiary data include information from textbooks, medical and nursing journals, drug handbooks, surveys, and policy and procedural manuals.
Methods of Data Collection
The main methods used to collect data are health interviews, physical examination, and observation.
The most common approach to gathering important information is through an interview. An interview is an intended communication or a conversation with a purpose, for example, to obtain or provide information, identify problems of mutual concern, evaluate change, teach, provide support, or provide counseling or therapy. One example of the interview is the nursing health history , which is a part of the nursing admission assessment. Patient interaction is generally the heaviest during the assessment phase of the nursing process so rapport must be established during this step.
Aside from conducting interviews, nurses will perform physical examinations, referencing a patient’s health history, obtaining a patient’s family history, and general observation can also be used to gather assessment data. Establishing a good physical assessment would, later on, provide a more accurate diagnosis, planning, and better interventions and evaluation .
Observation is an assessment tool that depends on the use of the five senses (sight, touch, hearing, smell, and taste ) to learn information about the client. This information relates to characteristics of the client’s appearance, functioning, primary relationships, and environment. Although nurses observe mainly through sight, most of the senses are engaged during careful observations such as smelling foul odors, hearing or auscultating lung and heart sounds and feeling the pulse rate and other palpable skin deformations.
Validation is the process of verifying the data to ensure that it is accurate and factual. One way to validate observations is through “double-checking,” and it allows the nurse to complete the following tasks:
- Ensures that assessment information is double-checked, verified, and complete. For example, during routine assessment, the nurse obtains a reading of 210/96 mm Hg of a client with no history of hypertension . To validate the data, the nurse should retake the blood pressure and if necessary, use another equipment to confirm the measurement or ask someone else to perform the assessment.
- Ensure that objective and related subjective data are valid and accurate. For example, the client’s perceptions of “feeling hot” need to be compared with the measurement of the body temperature.
- Ensure that the nurse does not come to a conclusion without adequate data to support the conclusion. A nurse assumes tiny purple or bluish-black swollen areas under the tongue of an older adult client to be abnormal until reading about physical changes of aging.
- Ensure that any ambiguous or vague statements are clarified. For example, a 86-year-old female client who is not a native English speaker says that “I am in pain on and off for 4 weeks,” would require verification for clarity from the nurse by asking “Can you describe what your pain is like? What do you mean by on and off?”
- Acquire additional details that may have been overlooked. For example, the nurse is asking a 32-year-old client if he is allergic to any prescription or non-prescription medications. And what would happen if he takes these medications.
- Distinguish between cues and inferences. Cues are subjective or objective data that can be directly observed by the nurse; that is, what the client says or what the nurse can see, hear, feel, smell, or measure. On the other hand, inferences are the nurse’s interpretation or conclusions made based on the cues. For example, the nurse observes the cues that the incision is red, hot, and swollen and makes an inference that the incision is infected.
Once all the information has been collected, data can be recorded and sorted. Excellent record-keeping is fundamental so that all the data gathered is documented and explained in a way that is accessible to the whole health care team and can be referenced during evaluation.
2. Diagnosis: “What is the problem?”
The second step of the nursing process is the nursing diagnosis . The nurse will analyze all the gathered information and diagnose the client’s condition and needs. Diagnosing involves analyzing data, identifying health problems, risks, and strengths, and formulating diagnostic statements about a patient’s potential or actual health problem. More than one diagnosis is sometimes made for a single patient. Formulating a nursing diagnosis by employing clinical judgment assists in the planning and implementation of patient care .
The types, components, processes, examples, and writing nursing diagnosis are discussed more in detail here “ Nursing Diagnosis Guide: All You Need To Know To Master Diagnosing ”
3. Planning: “How to manage the problem?”
Planning is the third step of the nursing process. It provides direction for nursing interventions . When the nurse, any supervising medical staff, and the patient agree on the diagnosis, the nurse will plan a course of treatment that takes into account short and long-term goals. Each problem is committed to a clear, measurable goal for the expected beneficial outcome.
The planning phase is where goals and outcomes are formulated that directly impact patient care based on evidence-based practice (EBP) guidelines. These patient-specific goals and the attainment of such assist in ensuring a positive outcome. Nursing care plans are essential in this phase of goal setting. Care plans provide a course of direction for personalized care tailored to an individual’s unique needs. Overall condition and comorbid conditions play a role in the construction of a care plan. Care plans enhance communication, documentation, reimbursement , and continuity of care across the healthcare continuum.
Types of Planning
Planning starts with the first client contact and resumes until the nurse-client relationship ends, preferably when the client is discharged from the health care facility.
Initial planning is done by the nurse who conducts the admission assessment. Usually, the same nurse would be the one to create the initial comprehensive plan of care.
Ongoing planning is done by all the nurses who work with the client. As a nurse obtain new information and evaluate the client’s responses to care, they can individualize the initial care plan further. An ongoing care plan also occurs at the beginning of a shift. Ongoing planning allows the nurse to:
- determine if the client’s health status has changed
- set priorities for the client during the shift
- decide which problem to focus on during the shift
- coordinate with nurses to ensure that more than one problem can be addressed at each client contact
Discharge planning is the process of anticipating and planning for needs after discharge. To provide continuity of care, nurses need to accomplish the following:
- Start discharge planning for all clients when they are admitted to any health care setting.
- Involve the client and the client’s family or support persons in the planning process.
- Collaborate with other health care professionals as needed to ensure that biopsychosocial, cultural, and spiritual needs are met.
A nursing care plan (NCP) is a formal process that correctly identifies existing needs and recognizes potential needs or risks. Care plans provide communication among nurses, their patients, and other healthcare providers to achieve health care outcomes. Without the nursing care planning process, the quality and consistency of patient care would be lost.
The planning step of the nursing process is discussed in detail in Nursing Care Plans (NCP): Ultimate Guide and Database .
4. Implementation: “Putting the plan into action!”
The implementation phase of the nursing process is when the nurse puts the treatment plan into effect. It involves action or doing and the actual carrying out of nursing interventions outlined in the plan of care. This typically begins with the medical staff conducting any needed medical interventions.
Interventions should be specific to each patient and focus on achievable outcomes. Actions associated with a nursing care plan include monitoring the patient for signs of change or improvement, directly caring for the patient or conducting important medical tasks such as medication administration, educating and guiding the patient about further health management, and referring or contacting the patient for a follow-up.
A taxonomy of nursing interventions referred to as the Nursing Interventions Classification (NIC) taxonomy, was developed by the Iowa Intervention Project. The nurse can look up a client’s nursing diagnosis to see which nursing interventions are recommended.
Nursing Interventions Classification (NIC) System
There are more than 550 nursing intervention labels that nurses can use to provide the proper care to their patients. These interventions are categorized into seven fields or classes of interventions according to the Nursing Interventions Classification system.
These are interventions designed to help a patient change their behavior. With behavioral interventions, in contrast, patient behavior is the key and the goal is to modify it. The following measures are examples of behavioral nursing interventions:
- Encouraging stress and relaxation techniques
- Providing support to quit smoking
- Engaging the patient in some form of physical activity , like walking , to reduce the patient’s anxiety , anger, and hostility
These are interventions that refer to the community-wide approach to health behavior change. Instead of focusing mainly on the individual as a change agent, community interventionists recognize a host of other factors that contribute to an individual’s capacity to achieve optimal health, such as:
- Implementing an education program for first-time mothers
- Promoting diet and physical activities
- Initiating HIV awareness and violence-prevention programs
- Organizing a fun run to raise money for breast cancer research
These are interventions that influence a patient’s entire family.
- Implementing a family-centered approach in reducing the threat of illness spreading when one family member is diagnosed with a communicable disease
- Providing a nursing woman support in breastfeeding her new baby
- Educating family members about caring for the patient
These are interventions that designed to maintain a safe medical facility for all patients and staff, such as:
- Following procedures to reduce the risk of infection for patients during hospital stays.
- Ensuring that the patient’s environment is safe and comfortable, such as repositioning them to avoid pressure ulcers in bed
These are interventions related to a patient’s physical health to make sure that any physical needs are being met and that the patient is in a healthy condition. These nursing interventions are classified into two types: basic and complex.
- Basic. Basic interventions regarding the patient’s physical health include hands-on procedures ranging from feeding to hygiene assistance.
- Complex. Some physiological nursing interventions are more complex, such as the insertion of an IV line to administer fluids to a dehydrated patient.
These are interventions that maintain a patient’s safety and prevent injuries, such as:
- Educating a patient about how to call for assistance if they are not able to safely move around on their own
- Providing instructions for using assistive devices such as walkers or canes, or how to take a shower safely.
When implementing care, nurses need cognitive, interpersonal, and technical skills to perform the care plan successfully.
- Cognitive Skills are also known as Intellectual Skills are skills involve learning and understanding fundamental knowledge including basic sciences, nursing procedures, and their underlying rationale before caring for clients. Cognitive skills also include problem-solving, decision-making, critical thinking, clinical reasoning, and creativity.
- Interpersonal Skills are skills that involve believing, behaving, and relating to others. The effectiveness of a nursing action usually leans mainly on the nurse’s ability to communicate with the patient and the members of the health care team.
- Technical Skills are purposeful “hands-on” skills such as changing a sterile dressing , administering an injection, manipulating equipment, bandaging, moving , lifting, and repositioning clients. All of these activities require safe and competent performance.
Process of Implementing
The process of implementing typically includes the following:
Prior to implementing an intervention, the nurse must reassess the client to make sure the intervention is still needed. Even if an order is written on the care plan, the client’s condition may have changed.
Other nursing tasks or activities may also be performed by non- RN members of the healthcare team. Members of this team may include unlicensed assistive personnel (UAP) and caregivers , as well as other licensed healthcare workers, such as licensed practical nurses/licensed vocational nurses (LPNs/LVNs). The nurse may need assistance when implementing some nursing intervention, such as ambulating an unsteady obese client, repositioning a client, or when a nurse is not familiar with a particular model of traction equipment needs assistance the first time it is applied.
3. Implementing the nursing interventions
Nurses must not only have a substantial knowledge base of the sciences, nursing theory, nursing practice , and legal parameters of nursing interventions but also must have the psychomotor skills to implement procedures safely. It is necessary for nurses to describe, explain, and clarify to the client what interventions will be done, what sensations to anticipate, what the client is expected to do, and what the expected outcome is. When implementing care, nurses perform activities that may be independent, dependent, or interdependent.
Nursing interventions are grouped into three categories according to the role of the healthcare professional involved in the patient’s care:
A registered nurse can perform independent interventions on their own without the help or assistance from other medical personnel, such as:
- routine nursing tasks such as checking vital signs
- educating a patient on the importance of their medication so they can administer it as prescribed
A nurse cannot initiate dependent interventions alone. Some actions require guidance or supervision from a physician or other medical professional, such as:
- prescribing new medication
- inserting and removing a urinary catheter
- providing diet
- Implementing wound or bladder irrigations
A nurse performs as part of collaborative or interdependent interventions that involve team members across disciplines.
- In some cases, such as post- surgery , the patient’s recovery plan may require prescription medication from a physician, feeding assistance from a nurse, and treatment by a physical therapist or occupational therapist.
- The physician may prescribe a specific diet to a patient. The nurse includes diet counseling in the patient care plan. To aid the patient, even more, the nurse enlists the help of the dietician that is available in the facility.
Delegate specific nursing interventions to other members of the nursing team as appropriate. Consider the capabilities and limitations of the members of the nursing team and supervise the performance of the nursing interventions. Deciding whether delegation is indicated is another activity that arises during the nursing process.
The American Nurses Association and the National Council of State Boards of Nursing (2006) define delegation as “the process for a nurse to direct another person to perform nursing tasks and activities.” It generally concerns the appointment of the performance of activities or tasks associated with patient care to unlicensed assistive personnel while retaining accountability for the outcome.
Nevertheless, registered nurses cannot delegate responsibilities related to making nursing judgments. Examples of nursing activities that cannot be delegated to unlicensed assistive personnel include assessment and evaluation of the impact of interventions on care provided to the patient.
Record what has been done as well as the patient’s responses to nursing interventions precisely and concisely.
5. Evaluation: “Did the plan work?”
Evaluating is the fifth step of the nursing process. This final phase of the nursing process is vital to a positive patient outcome. Once all nursing intervention actions have taken place, the team now learns what works and what doesn’t by evaluating what was done beforehand. Whenever a healthcare provider intervenes or implements care, they must reassess or evaluate to ensure the desired outcome has been met. The possible patient outcomes are generally explained under three terms: the patient’s condition improved, the patient’s condition stabilized, and the patient’s condition worsened.
Steps in Evaluation
Nursing evaluation includes (1) collecting data, (2) comparing collected data with desired outcomes, (3) analyzing client’s response relating to nursing activities, (4) identifying factors that contributed to the success or failure of the care plan, (5) continuing, modifying, or terminating the nursing care plan , and (6) planning for future nursing care.
The nurse recollects data so that conclusions can be drawn about whether goals have been fulfilled. It is usually vital to collect both objective and subjective data. Data must be documented concisely and accurately to facilitate the next part of the evaluating process.
The documented goals and objectives of the nursing care plan become the standards or criteria by which to measure the client’s progress whether the desired outcome has been met, partially met, or not met.
- The goal was met , when the client response is the same as the desired outcome.
- The goal was partially met , when either a short-term outcome was achieved but the long-term goal was not, or the desired goal was incompletely attained.
- The goal was not met.
It is also very important to determine whether the nursing activities had any relation to the outcomes whether it was successfully accomplished or not.
It is required to collect more data to confirm if the plan was successful or a failure. Different factors may contribute to the achievement of goals. For example, the client’s family may or may not be supportive, or the client may be uncooperative to perform such activities.
The nursing process is dynamic and cyclical. If goals were not sufficed, the nursing process begins again from the first step. Reassessment and modification may continually be needed to keep them current and relevant depending upon general patient condition. The plan of care may be adjusted based on new assessment data. Problems may arise or change accordingly. As clients complete their goals, new goals are set. If goals remain unmet, nurses must evaluate the reasons these goals are not being achieved and recommend revisions to the nursing care plan .
Discharge planning is the process of transitioning a patient from one level of care to the next. Discharge plans are individualized instructions provided as the client is prepared for continued care outside the healthcare facility or for independent living at home. The main purpose of a discharge plan is to improve the client’s quality of life by ensuring continuity of care together with the client’s family or other healthcare workers providing continuing care.
The following are the key elements of IDEAL discharge planning according to the Agency for Healthcare Research and Quality:
- I nclude the patient and family as full partners in the discharge planning process.
- Describe what life at home will be like
- Review medications
- Highlight warning signs and problems
- Explain test results
- Schedule follow-up appointments
- E ducate the patient and family in plain language about the patient’s condition, the discharge process, and next steps throughout the hospital stay.
- A ssess how well doctors and nurses explain the diagnosis, condition, and next steps in the patient’s care to the patient and family and use teach back.
- L isten to and honor the patient’s and family’s goals, preferences, observations, and concerns.
A discharge plan includes specific components of client teaching with documentation such as:
- Equipment needed at home. Coordinate home-based care and special equipment needed.
- Dietary needs or special diet . Discuss what the patient can or cannot eat at home.
- Medications to be taken at home. List the patient’s medications and discuss the purpose of each medicine, how much to take, how to take it, and potential side effects.
- Resources such as contact numbers and addresses of important people. Write down the name and contact information of someone to call if there is a problem.
- Emergency response: Danger signs. Identify and educate patients and families about warning signs or potential problems.
- Home care activities. Educate patient on what activities to do or avoid at home.
- Summary. Discuss with the patient and family about the patient’s condition, the discharge process, and follow-up checkups.
39 thoughts on “The Nursing Process: A Comprehensive Guide”
This article is helpful
So helpful And easy to understand A very good guide for nurses
I’m a clinical instructor teaching Fundamentals this semester. The article will be very helpful to give an in-depth explanation of “The Nursing Process” to students. Thank you.
Very detailed and easy to understand. Thx
Am a student I find it very educative
This is so helpful
Excellent information that is clearly outlined and user friendly.
This is so wonderful thank you
So helpful thank you
this is very helpful thank you
Helpful. So grateful
Is the nursing process the same as “critical thinking”?
Great information! Thanks!
This is very helpful. Thank you
Great explanation, in the understanding of Nursing process
Very Helpful to students, thank you for sharing
Excellent job. A great help to all nursing students. Thank you for sharing. God bless you.
Hi Joycelyn, Thank you so much for your kind words! It’s really rewarding to hear that it’s helping nursing students out there. We’re all about sharing knowledge and making things a bit easier. 😊 If there’s anything else you’d like to see or know, just let me know. And blessings right back at you!
Thank you so much…It’s a very comprehensive reference.
You’re very welcome, A.C! I’m glad you found the nursing process reference comprehensive and useful. Just out of curiosity, is there a particular step in the nursing process you’d like to explore more deeply, or do you have any specific areas where you’d like more detailed information?
I am a nursing student and I see this as a helpful tool, very detailed and easy to understand thanks for sharing
Hi Mawuli, I’m delighted to know that you’re finding our resources helpful! If you have any specific questions or if there’s a particular topic you’d like more information on, please feel free to ask. I’m here to assist you with any nursing-related inquiries you may have. Keep up the great work in your studies! 🩺📚🌟
Keep updating me about Nursing pdfs. You guys are really good at your work!!
Hey Mokete, Thank you so much for the kind words! We’re thrilled to hear that you’re finding our nursing resources helpful. We’ll do our best to keep you updated with more valuable nursing PDFs and information. If there’s anything specific you’d like to see or if you have any questions, feel free to let us know. Keep up the great work in your nursing journey! 👩⚕️📚🌟
Thanks it really helps alot
Glad to be of help! Thank you!
This guideline very useful for Nurses building their competency and practice quality of care of Nursing to use as reference please allow to download free especially to Nurses who live in developing countries since it is not affordable to buy it
You can download the articles by printing them as PDF :) You can use a service called printfriendly (google it) to make PDFs of our webpages.
Excellent work done I’m very happy to see this stuffs
Thank you so much…It’s a very comprehensive reference. God bless you
Hello Theophilus, You’re very welcome, and thank you for the blessings! 😊 I’m glad you found the reference on the nursing process comprehensive. Just out of curiosity, is there a particular part of the nursing process you’re most interested in, or any aspect you’d like to explore more deeply?
God bless you too, and if you have any more questions, feel free to ask!
Very helpful information. Thank you.
Thank you so much, Alisa. If you need more information or help regarding this, let us know.
You’re doing a great job here. Please can you do it in such a way for us to download it as a pdf?
Hi Millicent, Thank you so much for the kind words! 😊 I’m really glad you’re finding the site useful.
Regarding your request to download content as a PDF, a neat trick you can use is the “print” function in your web browser. Here’s how you can do it:
Open the page you want to save as a PDF. -Go to the “File” menu in your browser and select “Print,” or simply press Ctrl+P (Cmd+P on Mac). -In the print window, look for a destination option and select “Save as PDF” or something similar. -Adjust any settings as needed, then click “Save” or “Print,” and choose where you want to save the file on your computer.
This way, you can turn any page into a PDF for your personal use. If you have any more questions or need further assistance, feel free to ask. Always here to help!
Very helpful Thank you
Leave a Comment Cancel reply
Fastest Nurse Insight Engine
- MEDICAL ASSISSTANT
- Abdominal Key
- Anesthesia Key
- Basicmedical Key
- Otolaryngology & Ophthalmology
- Musculoskeletal Key
- Obstetric, Gynecology and Pediatric
- Oncology & Hematology
- Plastic Surgery & Dermatology
- Clinical Dentistry
- Radiology Key
- Thoracic Key
- Veterinary Medicine
- Gold Membership
Critical thinking, the nursing process, and clinical judgment
CHAPTER 8 Critical thinking, the nursing process, and clinical judgment Learning outcomes After studying this chapter, students will be able to: • Define critical thinking. • Describe the importance of critical thinking in nursing. • Contrast the characteristics of “novice thinking” with those of “expert thinking.” • Explain the purpose and phases of the nursing process. • Differentiate between nursing orders and medical orders. • Explain the differences between independent, interdependent, and dependent nursing actions. • Describe evaluation and its importance in the nursing process. • Define clinical judgment in nursing practice and explain how it is developed. • Devise a personal plan to use in developing sound clinical judgment. To enhance your understanding of this chapter, try the Student Exercises on the Evolve site at http://evolve.elsevier.com/Black/professional . Almost every encounter a nurse has with a patient is an opportunity for the nurse to assist the patient to a higher level of wellness or comfort. A nurse’s ability to think critically about a patient’s particular needs and how best to meet them will determine the extent to which a patient benefits from the nurse’s care. A nurse’s ability to use a reliable cognitive approach is crucial in determining a patient’s priorities for care and in making sound clinical decisions in addressing those priorities. This chapter explores several important and interdependent aspects of thinking and decision making in nursing: critical thinking, the nursing process, and clinical judgment. Chapter opening photo from istockphoto.com . Defining critical thinking Defining “critical thinking” is a complex task that requires an understanding of how people think through problems. Educators and philosophers struggled with definitions of critical thinking for several decades. Two decades ago, the American Philosophical Association published an expert consensus statement ( Box 8-1 ) describing critical thinking and attributes of the ideal critical thinker. This expert statement, still widely used, was the culmination of 3 years of work by Facione and others who synthesized the work of numerous persons who had defined critical thinking. More recently, Facione (2006) noted that giving a definition of critical thinking that can be memorized by the learner is actually antithetical to critical thinking! This means that the very definition of critical thinking does not lend itself to simplistic thinking and memorization. BOX 8-1 EXPERT CONSENSUS STATEMENT REGARDING CRITICAL THINKING AND THE IDEAL CRITICAL THINKER We understand critical thinking (CT) to be purposeful, self-regulatory judgment that results in interpretation, analysis, evaluation, and inference, as well as explanation of the evidential, conceptual, methodological, criteriological, or contextual considerations upon which that judgment is based. CT is essential as a tool of inquiry. As such, CT is a liberating force in education and a powerful resource in one’s personal and civic life. While not synonymous with good thinking, CT is a pervasive and self-rectifying human phenomenon. The ideal critical thinker is habitually inquisitive, well-informed, trustful of reason, open-minded, flexible, fair-minded in evaluation, honest in facing personal biases, prudent in making judgments, willing to reconsider, clear about issues, orderly in complex matters, diligent in seeking relevant information, reasonable in the selection of criteria, focused in inquiry, and persistent in seeking results that are as precise as the subject and the circumstances of inquiry permit. Thus educating good critical thinkers means working toward this ideal. It combines developing CT skills with nurturing those dispositions that consistently yield useful insights and that are the basis of a rational and democratic society. From American Philosophical Association : Critical Thinking: A Statement of Expert Consensus for Purposes of Educational Assessment and Instruction, The Delphi report: Research findings and recommendations prepared for the committee on pre-college philosophy, 1990, ERIC Document Reproduction Services, pp. 315–423. The Paul-Elder Critical Thinking Framework is grounded in this definition of critical thinking: “Critical thinking is that mode of thinking—about any subject, content, or problem—in which the thinker improves the quality of his or her thinking by skillfully taking charge of the structures inherent in thinking and imposing intellectual standards upon them.” Paul and Elder, 2012 Paul and Elder (2012) go on to describe a “well-cultivated critical thinker” as one who does the following: • Raises questions and problems and formulates them clearly and precisely • Gathers and assesses relevant information, using abstract ideas for interpretation • Arrives at conclusions and solutions that are well-reasoned and tests them against relevant standards • Is open-minded and recognizes alternative ways of seeing problems, and has the ability to assess the assumptions, implications, and consequences of alternative views of problems • Communicates effectively with others as solutions to complex problems are formulated We live in a “new knowledge economy” driven by information and technology that changes quickly. Analyzing and integrating information across an increasing number of sources of knowledge requires that you have flexible intellectual skills. Being a good critical thinker makes you more adaptable in this new economy of knowledge ( Lau and Chan, 2012). An excellent website on critical thinking can be found at http://philosophy.hku.hk/think/ (OpenCourseWare on critical thinking, logic, and creativity). So what does this have to do with nursing? The answer is very simple: excellent critical thinking skills are required for you to make good clinical judgments. You will be responsible and accountable for your own decisions as a professional nurse. The development of critical thinking skills is crucial as you provide nursing care for patients with increasingly complex conditions. Critical thinking skills provide you with a powerful means of determining patient needs, interpreting physician orders, and intervening appropriately. Box 8-2 presents an example of the importance of critical thinking in the provision of safe care. BOX 8-2 USING CRITICAL THINKING SKILLS TO IMPROVE A PATIENT’S CARE Ms. George has recently undergone bariatric surgery after many attempts to lose weight over the years have failed. She is to be discharged home on postoperative day 2, as per the usual protocol. Although she describes herself as “not feeling well at all,” the physician writes the order for discharge and you, as the nurse who does postoperative discharge planning for the surgery practice, prepare Ms. George to go home with her new dietary guidelines and encouragement for her successful weight loss. You note that Ms. George does not seem as comfortable or pleased with her surgery as most patients with whom you have worked in the past. Ms. George has to wait 3 hours for her husband to drive her home, and you note that she continues to lie on the bed passively, and her lethargy is increasing. You take her vital signs and note that her temperature is 37.8° C and her pulse is 115. You listen to her chest and note that it is difficult to appreciate breath sounds due to the patient’s body habitus. Ms. George points to an area just below her left breast where she notes pain with inspiration. You call her physician to report your findings; she responds that Ms. George’s pain is “not unusual” with her type of bariatric surgery and that her slightly increased temperature is “most likely” related to her being somewhat dehydrated. She instructs you to have Ms. George force fluids to the extent that she can tolerate it, and to take mild pain medication for postoperative pain. You ask her to consider delaying her discharge home, but she refuses. You give Ms. George acetaminophen as ordered, but her pain on inspiration continues. Her temperature remains at 37.8° C, and her pulse is 120. You measure her O 2 saturation with a pulse oximeter, and it is 91%. Her respirations are 26 and somewhat shallow. Her surgeon does not respond to your page, so you call the nursing supervisor, explaining to him that you are concerned with Ms. George’s impending discharge. Although you are wary of the surgeon’s reaction, you call the hospitalist (a physician who sees inpatients in the absence of their attending physician), who orders a chest x-ray study. Ms. George has evidence of a consolidation in her left lower lobe, which turns out to be a pulmonary abscess. She is treated on intravenous antibiotics for 5 days, and the abscess eventually has to be aspirated and drained. Your critical thinking skills and willingness to advocate for your patient prevented an even worse postoperative course. You recognized that Ms. George’s lethargy was unusual, and the location and timing of her pain was of concern. You also realized that although her temperature appeared to be stable, she had been given a pain medicine (acetaminophen) that also reduces fever, so in fact, a temperature increase may have been masked by the antipyretic properties of the acetaminophen. You demonstrated excellent clinical judgment in measuring her O 2 saturation. Furthermore, you sought support through the nursing “chain of command” when you engaged the nursing supervisor, who supported you in contacting the hospitalist. The specific, detailed information that you were able to provide the hospitalist allowed him to follow a logical diagnostic path, determining that Ms. George did indeed have a significant postoperative complication. Two days later, Ms. George reports that she is “feeling much better” and is walking in the hallways several times a day. Critical thinking in nursing You may be wondering at this point, “How am I ever going to learn how to make connections among all of the data I have about a patient?” This is a common response for a nursing student who is just learning some of the most basic psychomotor skills in preparation for practice. You need to understand that, just like learning to give injections safely and maintaining a sterile field properly, you can learn to think critically. This involves paying attention to how you think and making thinking itself a focus of concern. A nurse who is exercising critical thinking asks the following questions: “What assumptions have I made about this patient?” “How do I know my assumptions are accurate?” “Do I need any additional information?” and “How might I look at this situation differently?” Nurses just beginning to pay attention to their thinking processes may ask these questions after nurse–patient interactions have ended. This is known as reflective thinking. Reflective thinking is an active process valuable in learning and changing behaviors, perspectives, or practices. Nurses can also learn to examine their thinking processes during an interaction as they learn to “think on their feet.” This is a characteristic of expert nurses. As you move from novice to expert, your ability to think critically will improve with practice. In Chapter 6 you read about Dr. Patricia Benner (1984, 1996), who studied the differences in expertise of nurses at different stages in their careers, from novice to expert. So it is with critical thinking: novices think differently from experts. Box 8-3 summarizes the differences in novice and expert thinking. BOX 8-3 NOVICE THINKING COMPARED WITH EXPERT THINKING Novice nurses • Tend to organize knowledge as separate facts. Must rely heavily on resources (e.g., texts, notes, preceptors). Lack knowledge gained from actually doing (e.g., listening to breath sounds). • Focus so much on actions that they may not fully assess before acting • Need and follow clear-cut rules • Are often hampered by unawareness of resources • May be hindered by anxiety and lack of self-confidence • Tend to rely on step-by-step procedures and follow standards and policies rigidly • Tend to focus more on performing procedures correctly than on the patient’s response to the procedure • Have limited knowledge of suspected problems; therefore they question and collect data more superficially or in a less focused way than more experienced nurses • Learn more readily when matched with a supportive, knowledgeable preceptor or mentor Expert nurses • Tend to store knowledge in a highly organized and structured manner, making recall of information easier. Have a large storehouse of experiential knowledge (e.g., what abnormal breath sounds sound like, what subtle changes look like). • Assess and consider different options for intervening before acting • Know which rules are flexible and when it is appropriate to bend the rules • Are aware of resources and how to use them • Are usually more self-confident, less anxious, and therefore more focused than less experienced nurses • Know when it is safe to skip steps or do two steps together. Are able to focus on both the parts (the procedures) and the whole (the patient response). • Are comfortable with rethinking a procedure if patient needs require modification of the procedure • Have a better idea of suspected problems, allowing them to question more deeply and collect more relevant and in-depth data • Analyze standards and policies, looking for ways to improve them • Are challenged by novices’ questions, clarifying their own thinking when teaching novices From Alfaro-LeFevre R: Critical Thinking in Nursing: A Practical Approach, ed. 2, Philadelphia, 1999, Saunders. Reprinted with permission. Critical thinking is a complex, purposeful, disciplined process that has specific characteristics that make it different from run-of-the-mill problem solving. Critical thinking in nursing is undergirded by the standards and ethics of the profession. Consciously developed to improve patient outcomes, critical thinking by the nurse is driven by the needs of the patient and family. Nurses who think critically are engaged in a process of constant evaluation, redirection, improvement, and increased efficiency. Be aware that critical thinking involves far more than stating your opinion. You must be able to describe how you came to a conclusion and support your conclusions with explicit data and rationales. Becoming an excellent critical thinker is significantly related to increased years of work experience and to higher education level; moreover, nurses with critical thinking abilities tend to be more competent in their practice than nurses with less well-developed critical thinking skills ( Chang , Chang, Kuo et al., 2011). Box 8-4 summarizes these characteristics and offers an opportunity for you to evaluate your progress as a critical thinker. BOX 8-4 SELF-ASSESSMENT: CRITICAL THINKING Directions: Listed below are 15 characteristics of critical thinkers. Mark a plus sign (+) next to those you now possess, mark IP (in progress) next to those you have partially mastered, and mark a zero (0) next to those you have not yet mastered. When you are finished, make a plan for developing the areas that need improvement. Share it with at least one person, and report on progress weekly. Characteristics of critical thinkers: How do you measure up? ______ Inquisitive/curious/seeks truth ______ Self-informed/finds own answers ______ Analytic/confident in own reasoning skills ______ Open-minded ______ Flexible ______ Fair-minded ______ Honest about personal biases/self-aware ______ Prudent/exercises sound judgment ______ Willing to revise judgment when new evidence warrants ______ Clear about issues ______ Orderly in complex matters/organized approach to problems ______ Diligent in seeking information ______ Persistent ______ Reasonable ______ Focused on inquiry An excellent continuing education (CE) self-study module designed to improve your ability to think critically can be found online ( www.nurse.com/ce/CE168-60/Improving-Your-Ability-to-Think-Critically ). Continuing one’s education through lifelong learning is an excellent way to maintain and enhance your critical thinking skills. The website www.nurse.com has more than 500 CE opportunities available online and may be helpful to you as you seek to increase your knowledge base and improve your clinical judgment. Being intentional about improving your critical thinking skills ensures that you bring your best effort to the bedside in providing care for your patients. The nursing process: An intellectual standard Critical thinking requires systematic and disciplined use of universal intellectual standards ( Paul and Elder, 2012). In the practice of nursing, the nursing process represents a universal intellectual standard by which problems are addressed and solved. The nursing process is a method of critical thinking focused on solving patient problems in professional practice. The nursing process is “a conceptual framework that enables the student or the practicing nurse to think systematically and process pertinent information about the patient” ( Huckabay , 2009, p. 72). Humans are involved in problem solving on a daily basis. Suppose your favorite band is performing in a nearby city the night before your big exam in pathophysiology. Your exam counts 35% of your final grade. But you have wanted to see this band since you were 15, and you do not know when you will have another chance. You are faced with weighing a number of factors that will influence your decision about whether to go see the band: your grade going into the exam; how late you will be out the night before the exam; how far you will have to drive to see the band; and how much study time you will have to prepare for the exam in advance. You are really conflicted about this, so you decide to let another factor determine what you will do: the cost of the ticket. When you learn that the only seats available are near the back of the venue and cost $105.00 each, you decide to stay home, get a good night’s sleep before the big exam, and make a 98%. You then realize that with such a good grade on this exam, you will have much less pressure when studying for the final exam at the end of the semester. You have identified a problem (not a particularly serious one, but one with personal significance!), considered various factors related to the problem, identified possible actions, selected the best alternative, evaluated the success of the alternative selected, and made adjustments to the solution based on the evaluation. This is the same general process nurses use in solving patient problems through the nursing process. For individuals outside the profession, nursing is commonly and simplistically defined in terms of tasks nurses perform. Many students get frustrated with activities and courses in nursing school that are not focused on these tasks, believing themselves that the tasks of nursing are nursing. Even within the profession, the intellectual basis of nursing practice was not articulated until the 1960s, when nursing educators and leaders began to identify and name the components of nursing’s intellectual processes. This marked the beginning of the nursing process. In the 1970s and 1980s, debate about the use of the term “diagnosis” began. Until then, diagnosis was considered to be within the scope of practice of physicians only. Although nurses were not educated or licensed to diagnose medical conditions in patients, nurses recognized that there were human responses amenable to independent nursing intervention. A nursing diagnosis, then, is “a clinical judgment about individual, family or community responses to actual or potential health problems or life processes which provide the basis for selection of nursing interventions to achieve outcomes for which the nurse has accountability” (NANDA-I, 2012). These responses could be identified (diagnosed) through the careful application of specific defining characteristics. In 1973, the National Group for the Classification of Nursing Diagnosis published its first list of nursing diagnoses. This organization, which recently celebrated its 40th year, is now known as NANDA International (NANDA-I; NANDA is the acronym for North American Nursing Diagnosis Association). Its mission is to “facilitate the development, refinement, dissemination and use of standardized nursing diagnostic terminology” with the goal to “improve the health care of all people” (NANDA-I, 2012). In 2011, NANDA-I published its 2012–2014 edition of Nursing Diagnoses: Definitions and Classifications. Currently, NANDA-I has more than 200 diagnoses approved for clinical testing and has recently added 16 new diagnoses and 8 revised diagnoses. Diagnoses are also retired if it becomes evident that their usefulness is limited or outdated, such as the former diagnosis “disturbed thought processes.” Here is a simple example of how an approved nursing diagnosis may be used: Two days after a surgery for a large but benign abdominal mass, Mr. Stevens has not yet been able to tolerate solid food and has diminished bowel sounds. His abdomen is somewhat distended. Your diagnosis is that Mr. Stevens has dysfunctional gastrointestinal motility. This diagnosis is based on NANDA-I’s taxonomy because you have determined that the risk factors and physical signs and symptoms associated with this diagnosis apply to him. A more detailed discussion of nursing diagnosis is located in the next section of this chapter. The nursing process as a method of clinical problem solving is taught in schools of nursing across the United States, and many states refer to it in their nurse practice acts. The nursing process has sometimes been the subject of criticism among nurses. In recent years, some nursing leaders have questioned the use of the nursing process, describing it as linear, rigid, and mechanistic. They believe that the nursing process contributes to linear thinking and stymies critical thinking. They are concerned that the nursing process format, and rigid faculty adherence to it, encourages students to copy from published sources when writing care plans, thus inhibiting the development of a holistic, creative approach to patient care ( Mueller , Johnston, and Bligh, 2002). Certainly the nursing process can be taught, learned, and used in a rigid, mechanistic, and linear manner. Ideally the nursing process is used as a creative approach to thinking and decision making in nursing. Because the nursing process is an integral aspect of nursing education, practice, standards, and practice acts nationwide, learning to use it as a mechanism for critical thinking and as a dynamic and creative approach to patient care is a worthwhile endeavor. Despite reservations among some nurses about its use, the nursing process remains the cornerstone of nursing standards, legal definitions, and practice and, as such, should be well understood by every nurse. Phases of the nursing process Like many frameworks for thinking through problems, the nursing process is a series of organized steps, the purpose of which is to impose some discipline and critical thinking on the provision of excellent care. Identifying specific steps makes the process clear and concrete but can cause nurses to use them rigidly. Keep in mind that this is a process, that progression through the process may not be linear, and that it is a tool to use, not a road map to follow rigidly. More creative use of the nursing process may occur by expert nurses who have a greater repertoire of interventions from which to select. For example, if a newly hospitalized patient is experiencing a great deal of pain, a novice nurse might proceed by asking family members to leave so that he or she can provide a quiet environment in which the patient may rest. An expert nurse would realize that the family may be a source of distraction from the pain or may be a source of comfort in ways that the nurse may not be able to provide. The expert nurse, in addition to assessing the patient, is willing to consider alternative explanations and interventions, enhancing the possibility that the patient’s pain will be relieved. Phase 1: Assessment Assessment is the initial phase or operation in the nursing process. During this phase, information or data about the individual patient, family, or community are gathered. Data may include physiological, psychological, sociocultural, developmental, spiritual, and environmental information. The patient’s available financial or material resources also need to be assessed and recorded in a standard format; each institution usually has a slightly different method of recording assessment data. Types of data Nurses obtain two types of data about and from patients: subjective and objective. Subjective data are obtained from patients as they describe their needs, feelings, strengths, and perceptions of the problem. Subjective data are often referred to as symptoms. Examples of subjective data are statements such as, “I am in pain” and “I don’t have much energy.” The only source for these data is the patient. Subjective data should include physical, psychosocial, and spiritual information. Subjective data can be very private. Nurses must be sensitive to the patient’s need for confidence in the nurse’s trustworthiness. Objective data are the other types of data that the nurse will collect through observation, examination, or consultation with other health care providers. These data are measurable, such as pulse rate and blood pressure, and include observable patient behaviors. Objective data are often called signs. An example of objective data that a nurse might gather includes the observation that the patient, who is lying in bed, is diaphoretic, pale, and tachypneic, clutching his hands to his chest. Objective data and subjective data usually are congruent; that is, they usually are in agreement. In the situation just mentioned, if the patient told the nurse, “I feel like a rock is crushing my chest,” the subjective data would substantiate the nurse’s observations (objective data) that the patient is having chest pain. Occasionally, subjective and objective data are in conflict. A stark example of incongruent subjective and objective data well-known to labor and delivery nurses is when a pregnant woman in labor describes ongoing fetal activity (subjective data); however, there are no fetal heart tones (objective data), and the infant is stillborn. Incongruent objective and subjective data require further careful assessment to ascertain the patient’s situation more completely and accurately. Sometimes incongruent data reveal something about the patient’s concerns and fears. To get a clearer picture of the patient’s situation, the nurse should use the best communication skills he or she possesses to increase the patient’s trust, which will result in more openness.
Share this:
- Click to share on Twitter (Opens in new window)
- Click to share on Facebook (Opens in new window)
Related posts:
- The education of nurses: On the leading edge of transformation
- Becoming a nurse: Defining nursing and socialization into professional practice
- Illness, culture, and caring: Impact on patients, families, and nurses
- Health care in the United States
Stay updated, free articles. Join our Telegram channel
Comments are closed for this page.

Full access? Get Clinical Tree

The Nursing Process
The common thread uniting different types of nurses who work in varied areas is the nursing process—the essential core of practice for the registered nurse to deliver holistic, patient-focused care. Assessment An RN uses a systematic, dynamic way to collect and analyze data about a client, the first step in delivering nursing care. Assessment includes not only physiological data, but also psychological, sociocultural, spiritual, economic, and life-style factors as well. For example, a nurse’s assessment of a hospitalized patient in pain includes not only the physical causes and manifestations of pain, but the patient’s response—an inability to get out of bed, refusal to eat, withdrawal from family members, anger directed at hospital staff, fear, or request for more pain mediation.
Diagnosis The nursing diagnosis is the nurse’s clinical judgment about the client’s response to actual or potential health conditions or needs. The diagnosis reflects not only that the patient is in pain, but that the pain has caused other problems such as anxiety, poor nutrition, and conflict within the family, or has the potential to cause complications—for example, respiratory infection is a potential hazard to an immobilized patient. The diagnosis is the basis for the nurse’s care plan.
Outcomes / Planning Based on the assessment and diagnosis, the nurse sets measurable and achievable short- and long-range goals for this patient that might include moving from bed to chair at least three times per day; maintaining adequate nutrition by eating smaller, more frequent meals; resolving conflict through counseling, or managing pain through adequate medication. Assessment data, diagnosis, and goals are written in the patient’s care plan so that nurses as well as other health professionals caring for the patient have access to it.
Implementation Nursing care is implemented according to the care plan, so continuity of care for the patient during hospitalization and in preparation for discharge needs to be assured. Care is documented in the patient’s record.
Evaluation Both the patient’s status and the effectiveness of the nursing care must be continuously evaluated, and the care plan modified as needed.
Item(s) added to cart
- Faculty Logins
- Student Portal
- COVID-19 Info
We’re enrolling for all classes! Email [email protected] for more information.
Indigenous Peoples Land Acknowledgement
Visit us on our social media pages! Facebook , Instagram , and Twitter
- About Our Programs
- Acupuncture
- Medical Massage Therapy
- Registered Nursing
- Practical Nursing
- Admission Requirements
- Returning Alumni
- About Financial Aid
5 Key Steps of the Nursing Process: A Comprehensive Guide
06 Apr, 2023 | By: AIAM Author
As a nurse, the well-being of your patients is your top priority. But how do you ensure that you’re providing the best possible care? By following the five essential steps of the nursing process, of course! From assessment to evaluation, each step plays a critical role in delivering comprehensive care that addresses not just the physical needs of your patients but their emotional and psychological needs as well.
In this guide, we’ll take a deep dive into each step of the nursing process, equipping you with the knowledge and skills you need to provide exceptional care and make a meaningful impact in the lives of your patients. So let’s get started!
What Is the Nursing Process?
The nursing process is a systematic, patient-centered approach that emphasizes the importance of thorough assessment, careful planning, and thoughtful evaluation.
The nursing process empowers nurses to provide individualized care tailored to each patient’s needs. By taking a collaborative approach involving the patient, their family, and other healthcare team members, nurses can achieve positive health outcomes and improve their patients’ overall quality of life.
So if you’re a nurse, embrace the nursing process with enthusiasm and confidence, knowing that it is an invaluable tool that can help you make a real difference in the lives of those under your care.
What is the purpose of the nursing process?

The nursing process aims to provide a systematic and patient-centered approach to delivering quality care that meets each patient’s needs. The nursing process helps nurses identify and address the complex needs of their patients by following a step-by-step framework that includes assessment, diagnosis, planning, implementation, and evaluation.
By using the nursing process, nurses can gather important information about their patients, identify potential problems, set priorities, develop care plans, implement interventions, and evaluate the effectiveness of the care provided.
The nursing process also promotes collaboration among healthcare professionals, patients, and their families and helps ensure that the care provided is consistent, safe, and of the highest quality. Ultimately, the nursing process aims to help nurses deliver comprehensive care that promotes positive health outcomes and improves their patients’ overall quality of life.
What are the characteristics of the nursing process?
The nursing process has several key characteristics, making it a practical framework for delivering quality care. These characteristics include:
- Patient-centered care: The nursing process prioritizes patients’ preferences, values, and beliefs and aims to provide individualized care tailored to their needs.
- Systematic and organized care: The nursing process follows a step-by-step framework that includes assessment, diagnosis, planning, implementation, and evaluation, ensuring that all aspects of care are considered.
- Evidence-based practice: The nursing process is grounded in evidence-based practices. Nurses use the latest research and best practices to ensure that the care provided is safe, effective, and of the highest quality.
- Collaborative work: The nursing process encourages open communication, shared decision-making, and teamwork to achieve positive health outcomes.
- Dynamic and ongoing care plan: The nursing process is dynamic and ongoing, meaning that it is continually updated and revised as the patient’s needs and health status change. It allows nurses to adapt their care plans and interventions to ensure the patient receives the best care possible.
What Are the 5 Nursing Process Steps?
Now you are informed that nurses can provide the best patient care thanks to the nursing process. But how does each step work? In the upcoming paragraphs, we’ll look at the five key steps of the nursing process and explore how each one plays a vital role in delivering quality care.
So, whether you’re a nursing student or simply curious about the care process, get ready to learn more!
1. Assessment

As the first step in the nursing process, assessment involves gathering information about the patient’s health status and needs. It includes physical, psychological, social, and spiritual assessments and considers the patient’s medical history, current medications, and any allergies they may have. By conducting a thorough assessment, nurses can identify potential health problems and determine the appropriate interventions to address them.
It’s important to note that during the assessment phase, the patient plays an active role in the process. Nurses should involve patients in the assessment by asking open-ended questions, actively listening to their concerns, and noting any symptoms or discomfort they are experiencing. This approach helps establish a trusting relationship between the nurse and the patient.
Patients may also provide valuable insights into their health status, lifestyle, and preferences, which can help nurses develop a more comprehensive understanding of their needs. Ultimately, involving the patient in the assessment process ensures that their care is individualized and aligned with their goals and expectations.
2. Diagnosis
The next step in the nursing process is diagnosis. Diagnosis involves analyzing the data collected during the assessment to identify any actual or potential health problems.
Nurses use their clinical judgment and critical thinking skills to interpret the data and develop a clear understanding of the patient’s health status. This step is vital as it sets the foundation for the next step.
3. Planning

Planning is the third step in the nursing process and involves developing a care plan. During this stage, nurses are responsible for setting goals and objectives, identifying interventions that will help achieve those goals, and determining the resources required to implement the plan.
It is essential to involve the patient and their family in the planning process to ensure the plan is patient-centered and reflects the patient’s needs and values. Such an approach can promote patient empowerment and encourage ownership in their care.
The care plan should be realistic and achievable based on the patient’s health status and available resources. A well-developed care plan ensures the patient receives the best possible care and achieves positive health outcomes.
4. Implementation
Implementation is the fourth step in the nursing process and involves carrying out the plan of care. Implementation includes:
- Administering medications
- Providing treatments and interventions
- Educating patients and their families about their health status and care plan
Nurses should ensure that the care provided is consistent with the plan of care and that the patient is actively involved in the process.
5. Evaluation
The final step in the nursing process is evaluation. During the last stage of the nursing process, nurses are responsible for assessing the effectiveness of the care plan and determining whether the patient’s goals and objectives have been effective.
Nurses should also evaluate any complications or side effects of the care provided and adjust the care plan as needed. Evaluation is an ongoing process that helps ensure that the patient receives the best possible care and achieves positive health outcomes.
The Bottom Line
In conclusion, the nursing process is a systematic and patient-centered approach to delivering quality care. By following the five essential steps of assessment, diagnosis, planning, implementation, and evaluation, nurses can ensure that they address all aspects of the patient’s health and deliver individualized care that meets their needs. So whether you’re a nursing student or a healthcare professional, understanding the nursing process is essential for exceptional patient care.
Subscribe to our newsletter for updates!
Request more information.
- Open access
- Published: 26 August 2024
Using a flipped teaching strategy in undergraduate nursing education: students’ perceptions and performance
- Shaherah Yousef Andargeery 1 ,
- Hibah Abdulrahim Bahri 2 ,
- Rania Ali Alhalwani 1 ,
- Shorok Hamed Alahmedi 1 &
- Waad Hasan Ali 1
BMC Medical Education volume 24 , Article number: 926 ( 2024 ) Cite this article
18 Accesses
Metrics details
Flipped teaching is an interactive learning strategy that actively engages students in the learning process. Students have an active role in flipped teaching as they independently prepare for the class. Class time is dedicated to discussion and learning activities. Thus, it is believed that flipped teaching promotes students’ critical thinking, communication, application of knowledge in real-life situations, and becoming lifelong learners. The aim of this study was to describe the students’ perception of flipped teaching as an innovative learning strategy. And to assess if there was a difference in students’ academic performance between those who participated in a traditional teaching strategy compared to those who participated in flipped teaching intervention.
A quasi-experimental design with intervention and control groups. A purposive sampling technique of undergraduate nursing students was used.
A total of 355 students participated in both groups, and 70 out of 182 students in the intervention group completed the survey. The students perceived a moderate level of effectiveness of the flipped teaching classroom as a teaching strategy. The result revealed that there is a statistically significant difference in the mean students’ scores for the intervention group (M = 83.34, SD = 9.81) and control group (M = 75.57, SD = 9.82).
Flipped teaching proves its effectiveness in improving students’ learning experience and academic performance. Also, students had a positive perception about flipped teaching as it allowed them to develop essential nursing competencies. Future studies must consider measuring the influence of flipped teaching on students’ ability to acquire nursing competencies, such as critical thinking and clinical reasoning.
Peer Review reports
The successful outcome of individualized nursing care of each patient depends on effective communication between nurses and patients. Therapeutic communication consists of an exchange of verbal and non-verbal cues. It is a process in which the professional nurse uses specific techniques to help patients better understand their conditions and promote patients’ open communication of their thoughts and feelings in an environment of mutual respect and acceptance [ 1 ]. Effective educational preparation, continuing practice, and self-reflection about one’s communication skills are all necessary for becoming proficient in therapeutic communication. Teaching therapeutic communication to nursing students explains the principles of verbal and non-verbal communication that can be emphasized through classroom presentation, discussion, case studies and role-play. It also helps them develop their ability to communicate effectively with patients, families, and other health care professionals. Nursing students should be able to critically think, conceptualizing, applying, analyzing, synthesizing, and evaluating information generated by observation, experience, reflection, reasoning, and communication. Utilizing a traditional teaching strategy can be a challenge to meet the previously stated requirements [ 2 ]. Therefore, nurse educators should adapt unique teaching methods to help students learn and participate in their own education.
The “flipped classroom” is a pedagogical approach that has gained popularity worldwide to foster active learning. Active learning is defined as instructional strategies that actively engage students in their learning. It requires them to do meaningful learning activities and reflect on their actions [ 3 ]. Flipped teaching is a teaching strategy that promotes critical thinking and the application of information learned outside of the classroom to real-world situations and solves problems within the classroom. It is used in a way that allows educators to deliver lectures by using technologies such as video, audio files, PowerPoint or other media. Thus, the students can read or study those materials on their own at home before attending the class. As a result, discussions and debates about the materials take place throughout the lecture time. Some of the main principles of flipped teaching are increasing interaction and communication between students and educators, allocating more time for content mastery and understanding, granting opportunities for closing gaps and development, creating opportunities for active engagement, and providing immediate feedback [ 4 , 5 ]. This teaching/learning methodology is supported by constructivism learning theory. A “problem-solving approach to learning” is how constructivism is frequently described. In which, it requires a shift in the nurse educator’s epistemic assumptions about the teaching-learning process. Constructivism requires nursing educators to take on the role of a learning facilitator who encourages collaboration and teamwork as well as guides the students in building their knowledge. The underlying assumptions of constructivism include the idea that learning occurs as a result of social interaction in which the student actively creates their own knowledge, while prior experiences serve as the foundation for the learning process. The “flipping classroom” reflects that approach, which integrates student-centered learning [ 6 ].
Flipped teaching approach has students learning before lectures, teaching the material to better use classroom time for cooperative learning. The discussed herein represents studies and case studies from primary through graduate schools. The literature indicated students did see value in this pedagogical approach. Most of the studies found that flipped teaching was associated with better understanding of the material learned, higher academic achievement/performance, and potentially improved psychosocial factors (self-esteem, self-efficacy) that are associated with learning. Interestingly, one article pointed out that non-didactic material used in flipped-teaching lead to an increase in performance and this did not happen with didactic material.
According to Jordan et al. [ 7 ], a flipped teaching is a methodology that was developed as a response to advancements and changes in society, pedagogical approaches, and rapid growth and advancement of technology; The flipped teaching was evolved from the peer instruction and just in time teaching approaches. Jordan and colleagues [ 7 ] state that independent learning happens outside the classroom prior to the lesson through instructional materials while classroom time is maximized to fosters an environment of collaborative learning. Qutob [ 8 ] states that flipped teaching enhances student learning and engagement and promotes greater independence for students.
Jordan et al. [ 7 ] studied the use of flipped teaching on the teaching of first- and fourth-year students’ discrete mathematics and graphs, models, and applications. Across all the classes studied (pilot, graph, model and application, practices, computer and business administration), students preferred flipped teaching compared to traditional teaching. According to Jordan et al. [ 7 ], the quality of the materials and exercises, and perceived difficulty of the course and material are important to student satisfaction with this method. Additionally, it was found that interactions with teachers and collaborative learning were positive. Likewise, Nguyen et al. [ 9 ] found students favorably perceive flipped teaching. This is especially true for those students who have an understanding that the method involves preparation and interaction and how these affect the outcomes. Vazquez and Chiang [ 10 ] discuss the lessons learned from observing two large Principles of Economics Classes at the University of Illinois; each class held 900 students. Vazquez and Chiang [ 10 ] found that the students preferred watching videos over reading the textbook. Secondly, students were better prepared after they watched pre-lecture videos compared to reading the textbook beforehand. The third finding involved the length of time pre-lecture work should take; the authors state pre-lecture work should be approximately 15 to 20 min of work ahead of each in-class session. The fourth finding is that the flipped teaching is a costly endeavor. Finally, it was found that having the students watch videos before the lectures reduced the time spent in class covering the material; the end result of this is students spend more time engaging in active learning than reviewing the material.
Qutob [ 8 ] studied the effects of flip teaching using two hematology courses. One of the courses was delivered using traditional teaching and the other course was flipped teaching. Qutob [ 8 ] found that students in the flipped course not only performed better on academic tasks, but also they had more knowledge and understanding of the material covered compared to those in the traditional format class. Additionally, Qutob [ 8 ] revealed that students in the flipped classroom found this style of learning is more beneficial than traditional teaching. Moreover, Florence and Kolski [ 11 ] found an improvement in high school students’ writing post-intervention. The authors further found that students were more engaged with the material and had a positive perception of the flipped model. Bahadur and Akhtar [ 12 ] conducted a meta-analysis of twelve research articles on flipped teaching; the studies demonstrated that students taught in the flip teaching classroom performed better academically and were more interactive and engaged in the material than students taught through traditional methods. Galindo-Dominguez [ 13 ] conducted a systematic review using 61 studies and found evidence for the effectiveness of this approach compared to other pedagogical approaches with regards to academic achievement, improved self-efficacy, motivation, engagement, and cooperativeness. Webb et al. [ 14 ] studied 127 students taking microeconomics and found the delivery of flipped material (didactic vs. non-didactic) influenced students’ improvements. They further found performance improvements for the students who attended flipped classes using non-didactic pre-class material. At the same time, Webb et al. [ 14 ] further found non-improvement associated with flipped classes that used didactic pre-class materials; these materials are akin to traditional lectures.
In the context of nursing education, flipped teaching strategy has demonstrated promising and effective results in enhancing student motivation, performance, critical thinking skills, and learning quality. The flipped teaching classrooms were associated with high ratings in teaching evaluations, increased course satisfaction, improved critical thinking skills [ 15 ], improved exam results and learning quality [ 16 ] and high levels of personal, teaching, and pedagogical readiness [ 17 ]. Another study showed that student performance motivation scores especially in extrinsic goal orientation, control beliefs, and self-efficacy for learning and performance were significantly higher in the flipped teaching classroom when compared to the traditional classroom strategy [ 16 ].
Regardless of these important findings, there have been limited studies published about the flipped teaching strategy in Saudi Arabia, particularly among nursing students. Therefore, implementing the flipped teaching strategy in a therapeutic communication course would be effective in academic performance and retention of knowledge. The flipped teaching method will fit best with the goals of a therapeutic communication course as both focus on active learning and student engagement. This approach is well-matched for a therapeutic communication course as it allows students to apply and practice the communication techniques and strategies, they have learned outside of class from the flipped teaching materials and freeing up class time for interactive and experiential activities. The filliped teaching method can provide opportunities for students to apply effective interpersonal communication skills in classes, provide more time to observe students practicing therapeutic communication techniques through role-play, group discussions, and case studies. It also allows instructors to refine and provide individualized feedback and offer real-time guidance to help students improve their interpersonal communication skills.
The current study aims to examine the students’ perception of a teaching innovation based on the use of the flipped teaching strategy in the therapeutic communication course. Further, to compare if there is a difference in students’ academic performance of students who participate in a traditional teaching strategy when compared with students who participate in flipped teaching intervention.
Students who participated in the intervention group perceived a high level of effectiveness of the flipped teaching classroom as a teaching/learning strategy.
There is a significant difference in the mean scores of students’ academic performance between students who participate in a traditional teaching strategy (control group) when compared with those students who participate in flipped teaching classroom (intervention group).
Design of the study
Quantitative method, quasi-experimental design was used in this study. This research study involves implementing a flipped teaching strategy (intervention) to examine the effectiveness of the flipped teaching among the participants in the intervention group and to examine the significant difference in the mean scores of the students’ performance between the intervention and control group.
College of Nursing at one of the educational universities located in Saudi Arabia.
A purposive sampling technique was conducted in this study. This sampling technique allows the researcher to target specific participants who have certain characteristics that are most relevant and informative for addressing the research questions. The advantages of the purposive sampling lie in gathering in-depth, detailed and contextual data from the most appropriate sources and ensure that the study captures a more comprehensive understanding of the concept of interest by considering different viewpoints [ 18 ]. Participants were eligible to participate in this study if they were (1) Enrolled in the undergraduate nursing programs (Nursing or Midwifery Programs) in the College Nursing; (2) Enrolled in Therapeutic Communication Course; (3) at least 18 years old or older. Participant’s data was excluded if 50% of the responses were incomplete. The sample size was calculated using G-Power. The required participants for recruitment to implement this study is 152 participants to reach a confidence level of 95% and a margin error of 5%.
Measurement
Demographic data including the participants’ age and GPA were collected from all the participants. Educational characteristics related to the flipped teaching were collected from the participants in the intervention group including the level of English proficiency, program enrollment, attending previous, attending previous course(s) that used flipped teaching strategy, time spent each week preparing for the lectures, time spent preparing for the course exams, and recommendation for applying flipped teaching in other classes.
The student’s perception of the effectiveness of the flipped teaching strategy was measured by a survey that focused on the effectiveness of flipped teaching. This data was collected only from the participants in the intervention group. The survey involves 14 items that used 5-point Likert-type scale (5 = strongly agree, 4 = agree, 3 = neutral, 2 = disagree and 1 = strongly disagree). The sum of the scores was calculated for the item, a high score indicates a high effectiveness of flipped teaching. The survey was developed by Neeli et al. [ 19 ] and the author was contacted to obtain permission to use the survey. The reliability of the scale was tested using Cronbach alpha, which was 0.91, indicating that the scale has an excellent reliability.
Also, student academic performance was measured for both the intervention and control groups though the average cumulative scores of the assessment methods of students who were enrolled in the Therapeutic Communication Course, given a total of 100. The students’ grades obtained in the course were calculated based grading structure of the Ministry of Education in Saudi Arabia (The Rules and Regulations of Undergraduate Study and Examination).
Ethical approval
Institutional Review Board (IRB) approval (No. 22-0860) was received before conducting the study. Participants were provided with information about the study and informed about the consent process. Informed consent to participate was obtained from all the participants in the study.
Intervention
Therapeutic communication course was taught face-to-face for students enrolled in the second year in the Bachelor of Science in Midwifery and Bachelor of Science in Nursing Programs. There were eight sections for the therapeutic communication course, two of them were under the midwifery program and the remaining (six sections) were under the nursing program. Each section was held once a week in a two-hour length for 10 weeks during the second semester of 2022. Students in all sections received the same materials, contents, and assessment methods, which is considered the traditional teaching strategy. The contents of the course included the following topics: introduction of communication, verbal and written communication, listening skills, non-verbal communication, nurse-patient relationship, professional boundaries, communication styles, effective communication skills for small groups, communication through nursing process, communication with special needs patient, health education and principles for empowering individuals, communication through technology, and trends and issues in therapeutic communication. The course materials, course objectives and learning outcomes, learning resources, and other supporting materials were uploaded to the electronic platform “Blackboard” (A Learning Management System) for all sections to facilitate students’ preparation during classes. The assessment methods include written mid-term examination, case studies, group presentation, and final written examination. The grading scores for each assessment method were also the same for all sections.
The eight course sections were randomly assigned into traditional teaching strategy (control group) or flipped teaching strategy (intervention group). Figure 1 shows random distribution of the course sections. The intervention group ( n = 182) included one section of the Bachelor of Science in Midwifery program ( n = 55 students) and three sections of Bachelor of Science in Nursing program ( n = 127 students). The control group ( n = 173) included one section of the Bachelor of Science in Midwifery program ( n = 50 students) and three sections of Bachelor of Science in Nursing program ( n = 123 students). Although randomization of the participants is not possible, we were able to create comparison groups between participants who received the flipped teaching and traditional teaching strategy. To ensure the consistency of the information given to the students and reduce the variability, the instructors were meeting periodically and reviewed the materials together. More importantly, all students received the same topics and assessment methods as stated in the course syllabus and as mentioned above. The instructors in all sections were required to answer students’ questions, provide clarification to the points raised throughout the semester, and give constructive feedback after the evaluation of each assessment method. Students were encouraged to freely express their opinions on the issues discussed and to share their thoughts when the opinions were inconsistent.

Random Distribution of the Course Sections
The intervention group were taught the course contents by using the flipped teaching strategy. The participants in the intervention group were asked to read the lectures and watch short videos from online sources before coming to classes. Similar materials and links were uploaded by the course instructors into the Blackboard system. During the classes, participants were divided into groups and were given time to appraise research articles and case scenarios related to the topics of the course. During the discussion time, each group presented their answers, and the course instructors encouraged the students to share their thoughts and provided constructive feedback. Questions corresponded to the intended objectives and learning outcomes were posted during the class time in Kahoot and Nearpod platforms as a competition to enhance students’ engagement. By the end of the semester, the flipped teaching survey was electronically distributed to students who were involved in the intervention group to examine the educational characteristics and assess the students’ perceptions about the flipped teaching.
Data collection procedure
After obtaining the IRB approval, the PI sent invitation letters to the potential participants using their official university email accounts. The invitation letter included a Microsoft Forms’ link with the description about the study, aim, research question, and sample size required to conduct the study. All students gave their permission to participate, and informed consent was obtained from them ( N = 355). The link also included questions related to age, GPA, and approval to use their scores from assessment methods for research purposes. The first part of data collection was obtained immediately after the therapeutic communication course was over. The average cumulative scores of all the assessment methods (out of 100) were calculated to measure the students’ academic performance for both the intervention and control groups.
The second part of data collection was conducted after the final exam of the therapeutic communication course ( n = 182). A Microsoft Forms link was sent to the participants in the intervention group only. It included questions related to educational characteristics and students’ perception of the effectiveness of flipped teaching. Students needed a maximum of 10 min to complete the study survey.
Data analysis
Data was analyzed using the SPSS version 27. Descriptive analysis was used to analyze the demographic and educational characteristics and perception of flipped teaching strategy. An independent t-test was implemented to compare the mean scores of the intervention and control groups to examine whether there is a statistically significance difference between both groups. A significance level of p < 0.05 was determined as statistical significance in this study.
The total number of students who enrolled in therapeutic communication course was 355 students. The intervention group included 182 students and the control group included 173 students. The mean age of all participants in the study was 19 years old (M = 19.56, SD = 1.19). The mean GPA was 3.53 (SD = 1.43). Of those enrolled in the intervention group, only 70 out of 182 students completed the survey. Table 1 represents the description of the educational characteristics of the participants in intervention group ( n = 70). Around 65% of the participants reported that their level of English proficiency is intermediate, and they were enrolled in the nursing program. Half of the students had precious courses that used flipped teaching strategy. About one-third of the students indicated that they spent less than 15 min each week preparing for lectures. Around 65% of the students stated that they spent more than 120 min preparing for the course exam. Half of the students gave their recommendation for applying flipped teaching strategy in other courses. The mean score of the students’ performance in Therapeutic Communication course who enrolled in the intervention group is 83.34 (SD = 9.81) and for those who were enrolled in the control group is 75.57 (SD = 9.82).
The students perceived a moderate level of effectiveness of the flipped teaching classroom as a teaching strategy (M = 3.49, SD = 0.69) (Table 2 ). The three highest items that improved students’ perception about the flipped teaching strategy were: flipped classroom session develops logical thinking (M = 3.77, SD = 0.99), followed by flipped classroom session provides extra information (M = 3.68, SD = 1.02), then flipped classroom session improves the application of knowledge (M = 3.64, SD = 1.04). The three lowest items perceived by the students were: Flipped classroom session should have allotted more time for each topic (M = 3.11, SD = 1.07), flipped classroom session requires a long time for preparation and conduction (M = 3.23, SD = 1.04), and flipped classroom session reduces the amount of time needed for study when compared to lectures (M = 3.26, SD = 1.07).
An independent sample T-test was implemented to compare the mean scores of the students’ academic performance between the intervention group ( n = 182) and control group ( n = 173) (Table 3 ). The results of Levene’s test for equality of variances ( p = 0.801) indicated that equal variances assumed, and the assumption of equal variances has not been violated. The significant level value (2-tailed) is p ≤ 0.001, indicating that there is a statistically significant difference in the mean scores of students’ academic performance for the intervention group (M = 83.34, SD = 9.81) and control group (M = 75.57, SD = 9.82). The magnitude of the differences in the means (Mean difference= -7.77%, CI: -10.02 to -5.52) is very small (Eta squared = 0.00035).
Flipped teaching is a learning strategy that engages students in the learning process allowing them to improve their academic performance and develop cognitive skills [ 20 ]. This study investigated the effect of implementing flipped teaching as an interactive learning strategy on nursing students’ performance. Also, the study examined students’ perceptions of integrating flipped teaching into their learning process. Flipped teaching is identified as an interactive teaching strategy that provides an engaging learning environment with immediate feedback allowing students to master the learning content [ 4 , 5 ]. Improvement in the student’s academic performance and development of learning competencies were expected outcomes. The flipped classroom approach aligns with the constructivist theory of education, which posits that students actively construct their own knowledge and understanding through engaging with the content and applying it in meaningful contexts. By providing pre-class materials (e.g., videos, readings) for students to engage with independently, the flipped classroom allows them to build a foundational understanding of the concepts before class, enabling them to actively participate in discussions, problem-solving, and collaborative activities during the class. By shifting the passive acquisition of knowledge to the pre-class phase and dedicating in-class time to active, collaborative, and problem-based learning, the flipped classroom approach creates an environment that fosters deeper understanding, the development of critical thinking and clinical reasoning skills as well as the ability to apply knowledge in clinical practice [ 21 ].
Effectiveness of the flipped teaching on students’ academic performance
The influence of flipped teaching on students’ academic performance was identified by evaluating students’ examination scores. The results of this study indicated that flipped teaching had a significant influence on students’ academic performance ( p = 0.000). This significant influence implies the positive effectiveness of flipped teaching on students’ academic performance (M = 83.34, SD = 9.81) compared to traditional classroom (M = 75.57, SD = 9.82). These results are in line with other researchers regarding improving students’ academic performance [ 7 , 8 , 9 , 10 ]. Qutob’s [ 8 ] study shows that flipped teaching positively influences students’ performance. Preparation for class positively influenced students’ academic performance. The flipped classroom approach is underpinned by the principles of constructivism. These principles emphasize the active role of students in constructing their own understanding of concepts and ideas, rather than passively receiving information [ 21 ].
In a traditional classroom, the teacher typically delivers content through lectures, and students are tasked with applying that knowledge through homework or in-class activities. However, this model often fails to engage students actively in the learning process. In contract,
Flipped classroom requires students to prepare for the class which allows them to be exposed to the learning material before the class. During class time, students are giving opportunities to interact with their classmates and instructors to discuss the learning topic which can positively influencing their academic performance later [ 7 , 9 ]. Furthermore, the flipped classroom approach aligns perfectly with the core tenets of constructivism. Its adherence to the constructivist 5E Instructional Model further demonstrates its grounding in this learning theory. The 5E model, which includes the phases of engagement, exploration, explanation, elaboration, and evaluation, provides a framework for facilitating the active construction of knowledge [ 22 ].
It first sparks student interest and curiosity about the concepts (engagement), then enables students to investigate and experiment with the ideas through hands-on activities and investigations (exploration). This is followed by opportunities for students to make sense of their explorations and construct their own explanations (explanation). The flipped classroom then allows students to apply their knowledge in new contexts, deepening their understanding (elaboration). Finally, the evaluation phase assesses student learning and provides feedback, completing the cycle of constructivist learning [ 22 ]. This alignment with the 5E model, along with the flipped classroom’s emphasis on active learning and create environment that nurtures deeper understanding, the development of higher-order thinking skills, and the ability to transfer learning to real-world contexts.
In this study, one third of the students indicated that the preparation time was less than fifteen minutes a week. According to Vazquez and Chiang [ 10 ], preparation time for classroom should be about 15 to 20 min for each topic. Preparation for class did not take much time but positively influenced students’ academic performance. Furthermore, preparation for class allows students to develop the skills to be independent learners [ 8 ]. Independence in learning develops continuous learning skills, such as long-life learning which is a required competency for nursing. Garcia et al. [ 22 ] found out that focusing on shifting teachers’ practices towards active learning approaches, such as the 5E Instructional Model, can have lasting, positive impacts on students’ conceptual understanding and learning.
Students’ perception of flipped teaching as a teaching strategy
Students’ perception of flipped teaching as a learning strategy was examined using a survey developed by Neeli et al. [ 19 ]. Students recognize flipped teaching as an effective teaching strategy (M = 3.49, SD = 0.69) that had a positive influence on their learning processes and outcomes. Several studies identified the positive influence of flipped teaching on students’ learning process and learning outcomes [ 8 , 19 ]. Flipped teaching provides a problem-based learning environment allowing students to develop clinical reasoning, critical thinking, and a deeper understanding of the subject [ 5 , 8 , 19 , 23 ]. The flipped teaching approach introduces students to the learning materials before class. Class time is then utilized for discussion, hands-on, and problem-solving activities to foster a deeper understanding of the studied subject [ 5 ]. Consequently, flipped teaching provides a problem-based learning environment as it encourages students to be actively engaged in the learning process, work collaboratively with their classmates, and apply previously learned knowledge and skills to solve a problem. The result of this study is consistent with the results from a systematic review conducted by Youhasan et al. [ 5 ]. Implementing flipped teaching in undergraduate nursing education provides positive outcomes on students’ learning experiences and outcomes and prepares them to deal with future challenges in their academic and professional activities [ 5 ].
Implications
The results from this study identified that flipped teaching has a significant influence on students’ academic performance. The results also indicated that students have positive perception of flipped teaching as an interactive learning strategy. Flipped teaching pedagogy could be integrated in nursing curriculum to improve the quality of education process and outcomes which will result in improving the students’ performance. Flipped teaching provides an interactive learning environment that enhances the development of essential nursing competencies, such as communication, teamwork, collaboration, life-long learning, clinical reasoning, and critical thinking. For example, flipped teaching allows students to develop communication skills throughout discussion in the classroom, and collaboration skills by working with their classmate and instructor. In this study, flipped teaching was implemented in a theoretical course (therapeutic communication course). This interactive learning strategy could also be applied in clinical and practice setting for effective and meaningful learning process and outcomes.
Strengths and limitations
This research study reveals the effectiveness of flipped teaching on students’ academic performance. This study used a quasi-experimental design with control and intervention groups to investigate the influence of flipped teaching on nursing education. Nevertheless, this study has limitations. One of the study’s limitations is the lack of randomization, thus causal association between the variables cannot be investigated. In addition, this study used a self-administered survey which may include respondents’ bias; thus, it may affect the results. Also, this study investigated students’ perceptions of flipped teaching as a learning strategy. The results from examining students’ perceptions indicated that students had a positive perception of flipped teaching as it allowed them to develop essential nursing competencies. This study did not focus on identifying and measuring competencies. Therefore, future studies must consider measuring the influence of flipped teaching on students’ ability to acquire nursing competencies, such as critical thinking and clinical reasoning.
Flipped teaching is an interactive learning strategy that depends on students’ preparation of the topic to be interactive learners in the learning environment. Interactive learning environment improves learning process and outcomes. This study indicated that flipped teaching has significant influence on students’ academic performance. Students perceived flipped teaching as a learning strategy that allowed them to acquire learning skills, such as logical thinking and application of knowledge. These skills allow students to have meaningful learning experience. Also, students could apply these skills in other learning content and/or environments, for example, in clinical. Thus, we believe that flipped teaching is an effective learning approach to be integrated in the nursing curriculum to enhance students’ learning experience.
Data availability
The datasets generated and/or analyzed during the current study are not publicly available due to data privacy but are available from the corresponding author on reasonable request.
Abbreviations
Institutional Review Board
Standard deviation
The level of marginal significance within a statistical test
Confidence Interval of the Difference
Figueiredo AR, Potra TS. Effective communication transitions in nursing care: a scoping review. Ann Med. 2019;51(sup1):201–201. https://doi.org/10.1080/07853890.2018.1560159 .
Article Google Scholar
O’Rae A, Ferreira C, Hnatyshyn T, Krut B. Family nursing telesimulation: teaching therapeutic communication in an authentic way. Teach Learn Nurs. 2021;16(4):404–9. https://doi.org/10.1016/j.teln.2021.06.013 .
Thai NTT, De Wever B, Valcke M. The impact of a flipped classroom design on learning performance in higher education: looking for the best blend of lectures and guiding questions with feedback. Computers Educ. 2017;107:113–26. https://doi.org/10.1016/j.compedu.2017.01.003 .
Özbay Ö, Çınar S. Effectiveness of flipped classroom teaching models in nursing education: a systematic review. Nurse Educ Today. 2021;104922–104922. https://doi.org/10.1016/j.nedt.2021.104922 . 102 (n. Issue).
Youhasan P, Chen Y, Lyndon M, Henning MA. Exploring the pedagogical design features of the flipped classroom in undergraduate nursing education: a systematic review. BMC Nurs. 2021;20(1):50–50. https://doi.org/10.1186/s12912-021-00555-w .
Barbour C, Schuessler JB. A preliminary framework to guide implementation of the flipped classroom method in nursing education. Nurse Educ Pract. 2019;34:36–42. https://doi.org/10.1016/j.nepr.2018.11.001 .
Jordan C, Magrenan A, Orcos L. Considerations about flip education in the teaching of advanced mathematics. Educational Sci. 2019;9(3):227.
Qutob H. Effect of flipped classroom approach in the teaching of a hematology course. PLoS ONE. 2022;17(4):1–8.
Nguyen B, Yu X, Japutra A, Chen C. Reverse teaching: exploring student perceptions of flip teaching. Act Learn High Educ. 2016;17(1):51–61.
Vazquez J, Chiang E. Flipping out! A case study on how to flip the principles of economics classroom. Int Adv Econ Res. 2015;21(4):379–90.
Florence E, Kolski T. Investigating the flipped classroom model in a high school writing course: action research to impact student writing achievement and engagement. TechTrends: Link Res Pract Improve Learn. 2021;65(6):1042–52.
Bahadur G, Akhtar Z. Effect of teaching with flipped classroom model: a meta-analysis. Adv Social Sci Educ Humanit Res. 2021;15(3):191–7.
Google Scholar
Galindo-Dominguez H. Flipped classroom in the educational system: Trend or effective pedagogical model compared to other methodologies? J Educational Technol Soc. 2021;24(3):44–60.
Webb R, Watson D, Shepherd C, Cook S. Flipping the classroom: is it the type of flipping that adds value? Stud High Educ. 2021;46(8):1649–63.
Barranquero-Herbosa M, Abajas-Bustillo R, Ortego-Maté C. Effectiveness of flipped classroom in nursing education: a systematic review of systematic and integrative reviews. Int J Nurs Stud. 2022;135:104327. https://doi.org/10.1016/j.ijnurstu.2022.104327 .
Lelean H, Edwards F. The impact of flipped classrooms in nurse education. Waikato J Educ. 2020;25:145–57.
Youhasan P, Chen Y, Lyndon M, Henning MA. Assess the feasibility of flipped classroom pedagogy in undergraduate nursing education in Sri Lanka: a mixed-methods study. PLoS ONE. 2021;16(11):e0259003. https://doi.org/10.1371/journal.pone.0259003 .
Harris AD, McGregor JC, Perencevich EN, Furuno JP, Zhu J, Peterson DE, Finkelstein J. The use and interpretation of quasi-experimental studies in medical informatics. J Am Med Inf Association: JAMIA. 2006;13(1):16–23. https://doi.org/10.1197/jamia.M1749 .
Neeli D, Prasad U, Atla B, Kukkala SSS, Konuku VBS, Mohammad A. (2019). Integrated teaching in medical education: undergraduate student’s perception.
Baloch MH, Shahid S, Saeed S, Nasir A, Mansoor S. Does the implementation of flipped Classroom Model improve the Learning Outcomes of Medical College Students? A single centre analysis. J Coll Physicians Surgeons–pakistan: JCPSP. 2022;32(12):1544–7.
Robertson WH. The Constructivist flipped Classroom. J Coll Sci Teach. 2022;52(2):17–22.
Garcia I, Grau F, Valls C, Piqué N, Ruiz-Martín H. The long-term effects of introducing the 5E model of instruction on students’ conceptual learning. Int J Sci Educ. 2021;43(9):1441–58.
Chu TL, Wang J, Monrouxe L, Sung YC, Kuo CL, Ho LH, Lin YE. The effects of the flipped classroom in teaching evidence based nursing: a quasi-experimental study. PLoS ONE. 2019;14(1):e0210606.
Download references
Acknowledgements
The authors are grateful for the facilities and other support given by Princess Nourah bint Abdulrahman University Researchers Supporting Project number (PNURSP2024R447), Princess Nourah bint Abdulrahman University, Riyadh, Saudi Arabia.
This research was funded by Princess Nourah bint Abdulrahman University Researchers Supporting Project number (PNURSP2024R447), Princess Nourah bint Abdulrahman University, Riyadh, Saudi Arabia
Author information
Authors and affiliations.
Nursing Management and Education Department, College of Nursing, Princess Nourah bint Abdulrahman University, P.O. Box 84428, Riyadh, 11671, Saudi Arabia
Shaherah Yousef Andargeery, Rania Ali Alhalwani, Shorok Hamed Alahmedi & Waad Hasan Ali
Medical-Surgical Nursing Department, College of Nursing, Princess Nourah bint Abdulrahman University, P.O. Box 84428, Riyadh, 11671, Saudi Arabia
Hibah Abdulrahim Bahri
You can also search for this author in PubMed Google Scholar
Contributions
Conceptualization, H.B, S.Y.A, W.A.; methodology, S.Y.A., S.H.A.; validation, S.Y.A.; formal analysis, S.Y.A.; resources, H.B, S.Y.A, W.A, R. A.; data curation, S.Y.A, S.H.A.; writing—original draft preparation, R.A, H.B, S.Y.A., S.H.A, W.A; writing—review and editing, R.A, H.B, S.Y.A, S.H.A, W.A; supervision, R.A, H.B, S.Y.A, S.H.A.; project administration, R.A, S.Y.A, S.H.A.; funding acquisition, S.Y.A. All authors have read and agreed to the published version of the manuscript.
Corresponding author
Correspondence to Hibah Abdulrahim Bahri .
Ethics declarations
Institutional review board.
Institutional Review Board (IRB) in Princess Nourah bint Abdulrahman University, approval No. (22-0860).
Informed consent
Informed consents were obtained from all study participants.
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note.
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License, which permits any non-commercial use, sharing, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if you modified the licensed material. You do not have permission under this licence to share adapted material derived from this article or parts of it. The images or other third party material in this article are included in the article’s Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by-nc-nd/4.0/ .
Reprints and permissions
About this article
Cite this article.
Andargeery, S.Y., Bahri, H.A., Alhalwani, R.A. et al. Using a flipped teaching strategy in undergraduate nursing education: students’ perceptions and performance. BMC Med Educ 24 , 926 (2024). https://doi.org/10.1186/s12909-024-05749-9
Download citation
Received : 26 February 2024
Accepted : 05 July 2024
Published : 26 August 2024
DOI : https://doi.org/10.1186/s12909-024-05749-9
Share this article
Anyone you share the following link with will be able to read this content:
Sorry, a shareable link is not currently available for this article.
Provided by the Springer Nature SharedIt content-sharing initiative
- Flipped teaching
- Active learning
- Teaching strategy
- Nursing education
- Undergraduate nursing education
BMC Medical Education
ISSN: 1472-6920
- General enquiries: [email protected]

COMMENTS
Critical Thinking and Clinical Reasoning. Nurses make decisions while providing patient care by using critical thinking and clinical reasoning. Critical thinking is a broad term used in nursing that includes "reasoning about clinical issues such as teamwork, collaboration, and streamlining workflow." [1] Using critical thinking means that nurses take extra steps to maintain patient safety ...
Critical thinking in nursing is invaluable for safe, effective, patient-centered care. You can successfully navigate challenges in the ever-changing health care environment by continually developing and applying these skills. Images sourced from Getty Images. Critical thinking in nursing is essential to providing high-quality patient care.
The following are examples of attributes of excellent critical thinking skills in nursing. 1. The ability to interpret information: In nursing, the interpretation of patient data is an essential part of critical thinking. Nurses must determine the significance of vital signs, lab values, and data associated with physical assessment.
Critical thinking is a cognitive process that involves analyzing, evaluating, and synthesizing information to make reasoned and informed decisions. It's a mental activity that goes beyond simple memorization or acceptance of information at face value. Critical thinking involves careful, reflective, and logical thinking to understand complex ...
Critical thinking is applied by nurses in the process of solving problems of patients and decision-making process with creativity to enhance the effect. It is an essential process for a safe, efficient and skillful nursing intervention. Critical thinking according to Scriven and Paul is the mental active process and subtle perception, analysis ...
Critical thinking is a multidimensional skill, a cognitive or mental process or set of procedures. It involves reasoning and purposeful, systematic, reflective, rational, outcome-directed thinking based on a body of knowledge, as well as examination and analysis of all available information and ideas. Critical thinking leads to the formulation ...
Successful nurses think beyond their assigned tasks to deliver excellent care for their patients. For example, a nurse might be tasked with changing a wound dressing, delivering medications, and monitoring vital signs during a shift. However, it requires critical thinking skills to understand how a difference in the wound may affect blood ...
Critical thinking is a complex, dynamic process formed by attitudes and strategic skills, with the aim of achieving a specific goal or objective. The attitudes, including the critical thinking attitudes, constitute an important part of the idea of good care, of the good professional. It could be said that they become a virtue of the nursing ...
Critical thinking in nursing involves the ability to question assumptions, analyze data, and evaluate outcomes. It's a disciplined process that includes observation, experience, reflection, reasoning, and communication. For nurses, critical thinking means being able to make sound clinical judgments that can significantly affect patient outcomes.
Critical thinking in nursing refers to the analytical process that nurses use to solve clinical problems and make decisions regarding patient care. It involves gathering information, questioning, analyzing, and applying theory to ensure high-quality care delivery. Nurse Education in Practice, 2022. About this page.
Critical thinking in nursing is an essential component of professional accountability and quality nursing care. ... in response to knowledge and as a trigger for action and/or reflection with a direct bearing on the analytical process involved in patient care. ... or modus operandi thinking, has characteristics of "critical reflection," but ...
Study with Quizlet and memorize flashcards containing terms like Critical thinking characteristics include a. Considering what is important in a given situation. ... ANS: D Using the nursing process along with applying components of the nursing critical thinking model will help the new graduate nurse make the most appropriate clinical decisions.
Critical thinking is an integral part of nursing, especially in terms of professionalization and independent clinical decision-making. It is necessary to think critically to provide adequate, creative, and effective nursing care when making the right decisions for practices and care in the clinical setting and solving various ethical issues ...
Skills. in critical thinking refer to the cognitive (intellectual) processes used in complex thinking operations such as problem-solving and decision making. When planning nursing care, nurses gather information about the client. and then draw tentative conclusions about the meaning of the information to identify the client's problems.
The nursing process is defined as a systematic, rational method of planning that guides all nursing actions in delivering holistic and patient-focused care. The nursing process is a form of scientific reasoning and requires the nurse's critical thinking to provide the best care possible to the client.
s, and problem-solving, which requires analysis. Decision-makingfree flow of ideas is essential to problem-solving and decision-making becaus. it helps prevent preconceived ideas from controlling the process. Many decisions in healthcare are arrived at by group or teams rather than by the in. vidual, and this type of decision-making requ.
The nursing process is a method of critical thinking focused on solving patient problems in professional practice. The nursing process is "a conceptual framework that enables the student or the practicing nurse to think systematically and process pertinent information about the patient" ( Huckabay, 2009, p. 72).
Critical thinking is an essential process for the safe, efficient and skillful nursing practice. ... Key Words: critical thinking, nursing education, clinical nurse education, clinical nursing practice doi: 10.5455/aim.2014.22.283-286 ... modify the emotions involved with critical thinking. So, if they feel anger, guilt and frustration for some ...
Care is documented in the patient's record. Evaluation. Both the patient's status and the effectiveness of the nursing care must be continuously evaluated, and the care plan modified as needed. Learn more about the nursing process, including its five core areas (assessment, diagnosis, outcomes/planning, implementation, and evaluation).
Chapter 6 - Nursing Process and Critical Thinking. NANDA I describes it as "human responses to health conditions/life processes that exists in an individual, family, or community. It is supported by defining characteristics (manifestations, signs and symptoms) that cluster in patterns of related cues or inferences.
The nursing process is a vital skill for nurses to provide safe, effective, and holistic patient care. Learn the 5 key steps of the nursing process—assess, diagnose, plan, implement, and evaluate—and how they can help you improve your clinical outcomes and patient satisfaction. This comprehensive guide from AIAM, a leading institute of alternative medicine and nursing education, will help ...
ANS: 2. Critical thinking and the nursing process are ways of thinking that can be used in problem solving (although critical thinking can be used beyond problem-solving applications). Neither method of thinking is linear. The nursing process has specific steps; critical thinking does not. PTS:1DIFgrinifficultREF: p. 31.
Flipped teaching is an interactive learning strategy that actively engages students in the learning process. Students have an active role in flipped teaching as they independently prepare for the class. Class time is dedicated to discussion and learning activities. Thus, it is believed that flipped teaching promotes students' critical thinking, communication, application of knowledge in real ...
Study with Quizlet and memorize flashcards containing terms like 1. Which of the following characteristics do the various definitions of critical thinking have in common? Critical thinking: a) Requires reasoned thought b) Asks the questions "why" or "how" c) Is a hierarchical process d) Demands specialized thinking skills, 2. A few nurses on a unit have proposed to the nurse manager that the ...
UNESCO